Why Finding Insurance That Covers Pre-Existing Conditions Matters More Than Ever
Insurance that covers pre-existing conditions is available to most Americans today — and in many cases, insurers cannot legally deny you or charge you more because of your health history.
Here’s a quick answer based on your situation:
| Insurance Type | Covers Pre-Existing Conditions? | Notes |
|---|---|---|
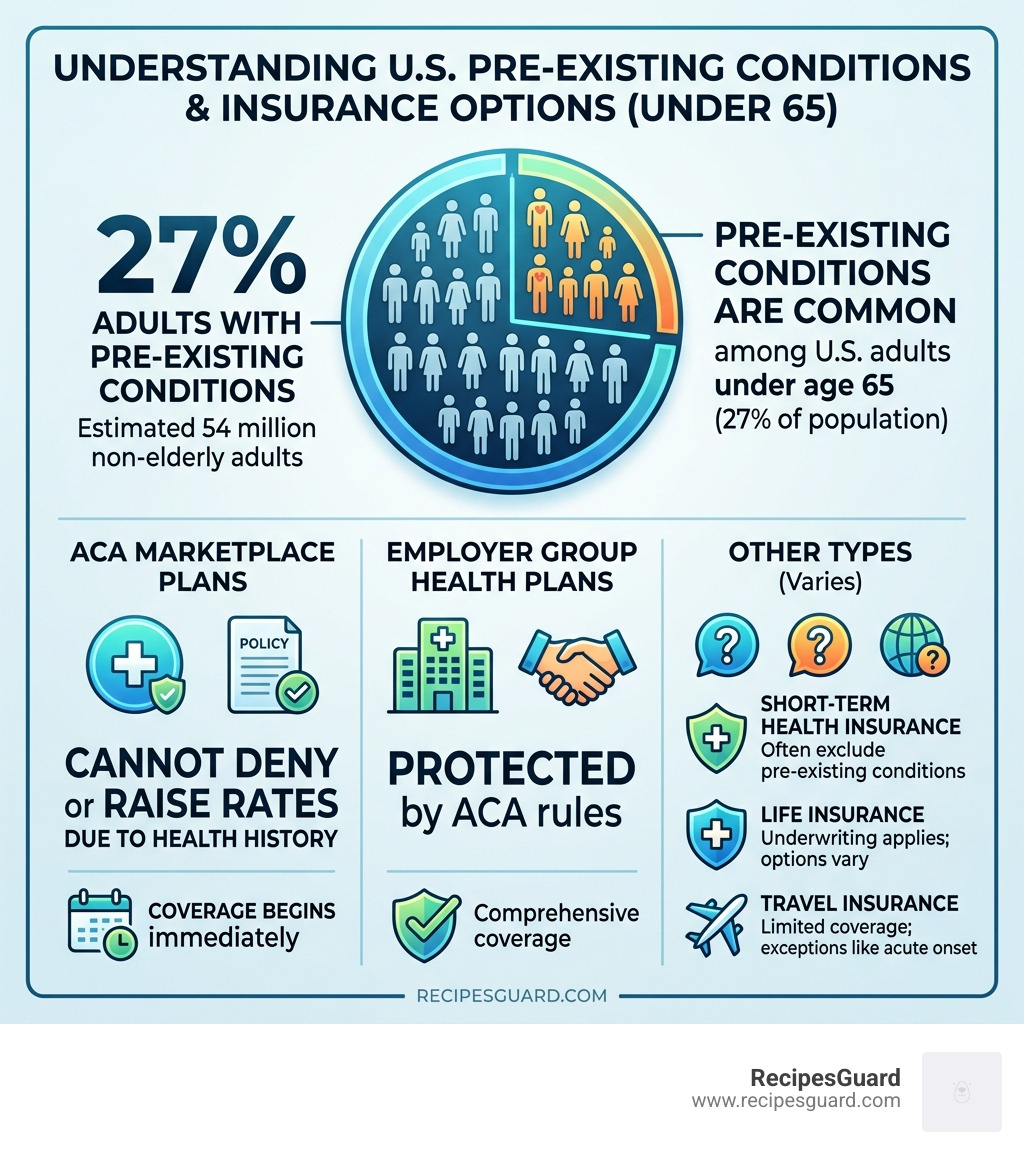
| ACA Marketplace plans | Yes | Cannot deny or raise rates |
| Employer group health plans | Yes | ACA-compliant protections apply |
| Grandfathered health plans | No | Exempt from ACA rules |
| Short-term health insurance | Often no | Not ACA-compliant |
| Life insurance | Varies | Underwriting applies; options exist |
| Travel / international insurance | Limited | “Acute onset” coverage may apply |
Before 2010, a diagnosis of asthma, diabetes, or even a past pregnancy could get your health insurance application rejected outright. Today, that has changed — significantly — for most plan types in the U.S.
Nearly 54 million Americans under age 65 have pre-existing health conditions. That’s 27% of all non-elderly adults. In other words, roughly 1 in 4 people reading this is directly affected.
But here’s where it gets complicated: not all insurance works the same way. Health insurance, life insurance, and travel insurance each handle pre-existing conditions very differently. And for international students navigating coverage abroad, the rules can feel like a maze.
This guide breaks it all down — clearly, step by step.
Insurance that covers pre existing terminology:
- Disability insurance that covers pre-existing conditions
- Family health insurance pre-existing condition
- Health insurance undiagnosed condition
Defining Pre-Existing Conditions in 2026

What exactly counts as a pre-existing condition? In the simplest terms, it is any health issue—chronic or acute—that you had before your new insurance coverage started. It doesn’t always have to be a major illness like cancer or heart disease. Even something as common as acne, anxiety, or high blood pressure can be flagged.
As of May 2026, nearly half of all Americans are living with at least one chronic health issue. When we talk about insurance that covers pre existing conditions, we are usually referring to:
- Chronic Illnesses: Diabetes, asthma, COPD, and sleep apnea.
- Serious Diagnoses: Cancer, heart disease, and lupus.
- Mental Health: Depression and anxiety disorders.
- Past Injuries: A broken leg or a surgery you had years ago (though these rarely affect health insurance today, they might still pop up on life insurance applications).
One nuance that often trips people up is the “Prudent Person Standard.” In some insurance contexts, a condition is considered pre-existing even if you haven’t been formally diagnosed. If you had symptoms that would cause a “prudent person” to seek medical advice, or if you simply asked your doctor about a recurring pain, an insurer might classify it as an existing condition.
To understand how these diagnoses interact with modern law, you can read A Deep Dive into Pre-Existing Conditions and Insurance. The good news is that for most of us, Why Your Family’s Medical History Won’t Break the Bank Anymore is the new reality thanks to consumer protection laws.
Health Insurance That Covers Pre-Existing Conditions Under the ACA
The Affordable Care Act (ACA) changed the game in 2010 (with full protections kicking in by 2014). We no longer live in a world where a “pre-existing condition exclusion period” can keep you from getting the care you need.
Under the ACA, insurance that covers pre existing conditions is the standard for almost all major medical plans. Insurers are prohibited from:
- Refusing coverage: They cannot turn you away because you have cancer or diabetes.
- Charging more: Your premiums are based on age, location, and tobacco use—not your health history.
- Excluding benefits: They cannot offer you a plan but refuse to pay for your insulin or chemotherapy.
This applies to all Marketplace plans and most employer-sponsored insurance. Furthermore, pregnancy is explicitly protected. If you are pregnant when you apply for a new plan, the insurer must cover your prenatal care and childbirth from day one.
For a deeper look at these rights, see Healthcare That Covers Pre-Existing Conditions: What You Need to Know.
| Feature | ACA-Compliant Plans | Grandfathered Plans |
|---|---|---|
| Covers Pre-Existing? | Yes, from day one | No, may exclude them |
| Can Deny Coverage? | No | Yes |
| Covers Pregnancy? | Yes, as an essential benefit | Not necessarily |
| Rate Hikes for Health? | Prohibited | Allowed |
Exceptions to Insurance That Covers Pre-Existing Conditions
While the ACA covers most bases, there are still “legacy” or “grandfathered” plans. These are plans that existed before March 23, 2010, and haven’t changed significantly. They are not required to follow ACA rules, meaning they can still deny coverage for pre-existing conditions.
Other exceptions include:
- Short-term health insurance: Designed for temporary gaps, these plans often have a “look-back period” and will not cover anything you’ve been treated for recently.
- Limited benefit policies: Such as hospital indemnity or dental-only plans.
If you find yourself stuck in a plan that doesn’t offer the protection you need, our Comprehensive Guide to ACA Protections and Plan Exceptions can help you navigate a transition.
How to Select the Best Marketplace Plan
If you have a chronic condition, “cheap” isn’t always “affordable.” We often recommend that people with high medical needs look at Gold or Platinum tier plans. While the monthly premiums are higher, the deductibles are much lower, which can save you thousands if you require regular specialist visits or expensive medications.
When comparing, always check the Summary Plan Description (SPD) to see if your specific drugs are covered in the specialty pharmacy section. You should also verify that your current doctors are in-network. For more tips on this, check out The Best Ways to Compare Health Insurance Coverage Today.
Life Insurance Options for Those with Medical Histories

Life insurance is a different beast entirely. Unlike health insurance, life insurance companies can and do use your medical history to decide if they will cover you and how much they will charge. This process is called medical underwriting.
When you apply, you’ll be placed into a “rate class.” If you have well-managed high blood pressure, you might still get a “Standard” or even “Preferred” rate. However, if you have unmanaged diabetes or a recent cancer diagnosis, you might be classified as “Substandard,” leading to much higher premiums.
If you’ve been denied traditional life insurance, don’t panic. You still have options:
- Guaranteed Issue Life Insurance: No medical exam and no health questions. These are more expensive and often have a “graded death benefit,” meaning if you pass away within the first two years, your beneficiaries might only receive the premiums you paid plus interest.
- Group Life Insurance: Many employers offer this as a benefit. It usually doesn’t require a medical exam, making it the easiest way to get insurance that covers pre existing conditions in the life insurance space.
To learn more about these nuances, see Navigating Life Insurance with Medical Histories and Don’t Let Your Medical History Stop Your Future Disability Coverage.
Improving Eligibility for Life Insurance That Covers Pre-Existing Conditions
Insurers love “manageability.” If you can prove that you are compliant with your doctor’s treatment plan—taking your medication, maintaining a healthy BMI, and having regular check-ups—you are a much lower risk.
Some people choose to wait until a condition has been stable for 6 to 12 months before applying to secure a better rate. If you improve your health significantly (like quitting smoking or losing weight) after your policy is active, you can often request a “re-rating” to lower your premiums. For a plan of action, follow our Step-by-Step: Improving Your Insurance Eligibility.
Navigating Travel and International Coverage Strategies
For students and travelers, the rules change again. Most travel medical insurance policies exclude pre-existing conditions by default. However, many offer a benefit called “Acute Onset of a Pre-Existing Condition.”
This covers a sudden, unexpected flare-up that requires emergency care. For example, if you have asthma and have a sudden, severe attack while hiking in the Blue Mountains, that might be covered. But routine check-ups for your asthma would not be.
Key terms to watch for:
- Stability Period: The insurer usually requires the condition to have been “stable” (no changes in medication or new symptoms) for 6 to 12 months before the trip.
- Look-back Period: How far back the insurer will check your medical records if you file a claim.
We dive deep into these strategies in Travel Insurance Strategies for Pre-Existing Conditions and our guide: Don’t Let Old Aches Break Your Travel Bank.
Finding Travel Insurance That Covers Pre-Existing Conditions
If you need full coverage for an existing condition while abroad, you may need a medical waiver. These are often available if you purchase your travel insurance within a short window (usually 14–21 days) of making your initial trip deposit.
For students, specifically those coming to or from Australia, ensure your Overseas Student Health Cover (OSHC) or international plan is robust. If you’re traveling without a formal diagnosis but have been feeling “off,” check out The Ultimate Guide to Holiday Insurance for People Without a Diagnosis Yet.
Frequently Asked Questions About Medical Coverage
Is pregnancy considered a pre-existing condition?
In ACA-compliant health insurance, yes, it is technically a pre-existing condition if it began before your coverage. However, the law mandates that it must be covered immediately. You cannot be denied, and you cannot be charged more. Furthermore, giving birth or adopting a child triggers a Special Enrollment Period, giving you 60 days to switch or buy a new plan.
Can I be denied coverage or charged more for a chronic illness?
If you are buying a plan on the Marketplace or getting insurance through a large employer, the answer is a firm no. Price discrimination based on health status is illegal for these plans. However, if you are looking at life insurance or short-term medical plans, they can still deny you or charge higher premiums based on your risk profile.
What was the Pre-Existing Condition Insurance Plan (PCIP)?
The PCIP was a temporary bridge program created by the ACA that ran from 2010 to 2014. It was funded with $5 billion to provide insurance to people who had been denied by private companies. States like California received large chunks of this funding ($761 million) to manage these high-risk pools. Today, the PCIP is no longer necessary because the Marketplace guarantees coverage for everyone.
Conclusion
At RecipesGuard, we know that navigating insurance that covers pre-existing conditions can feel like a full-time job. Whether you’re an international student trying to understand a claim or a family looking for the right Marketplace tier, the most important step is honesty. Disclosing your history ensures that when you do file a claim, it actually gets paid.
We specialize in providing student-focused, step-by-step claim filing tutorials. If you’re worried about how your medical history might affect your future, we’re here to help you navigate the paperwork so you can focus on your health.
Learn more about our mission and services

My name is Bianca, and my journey into the world of fermentation and food safety began with a costly mistake. I once lost an entire season’s harvest of chili peppers because I relied on guesswork instead of science. That failure was my turning point.

