Healthcare That Covers Pre-Existing Conditions: What You Need to Know
What You Need to Know About Medical Aid That Covers Pre-Existing Conditions
Medical aid that covers pre existing conditions exists in both the US and South Africa, but the rules are very different depending on where you are.
Here’s a quick overview:
| Location | Coverage Rule | Waiting Period |
|---|---|---|
| US (ACA Marketplace) | Must cover all pre-existing conditions | No waiting period |
| US (Grandfathered plans) | May deny or charge more | Varies |
| South Africa (medical aid) | Cannot refuse membership, but can exclude conditions | 3–12 months |
| Travel insurance | May cover with a waiver | 120-day look-back period |
A pre-existing condition is any health issue you had before your new coverage started. This includes:
- Chronic conditions like diabetes, asthma, or hypertension
- Past injuries or surgeries
- Mental health conditions like depression or anxiety
- Even pregnancy, in some systems
Whether you’re an international student abroad or someone managing a long-term illness, understanding your rights can mean the difference between a covered claim and a costly surprise.
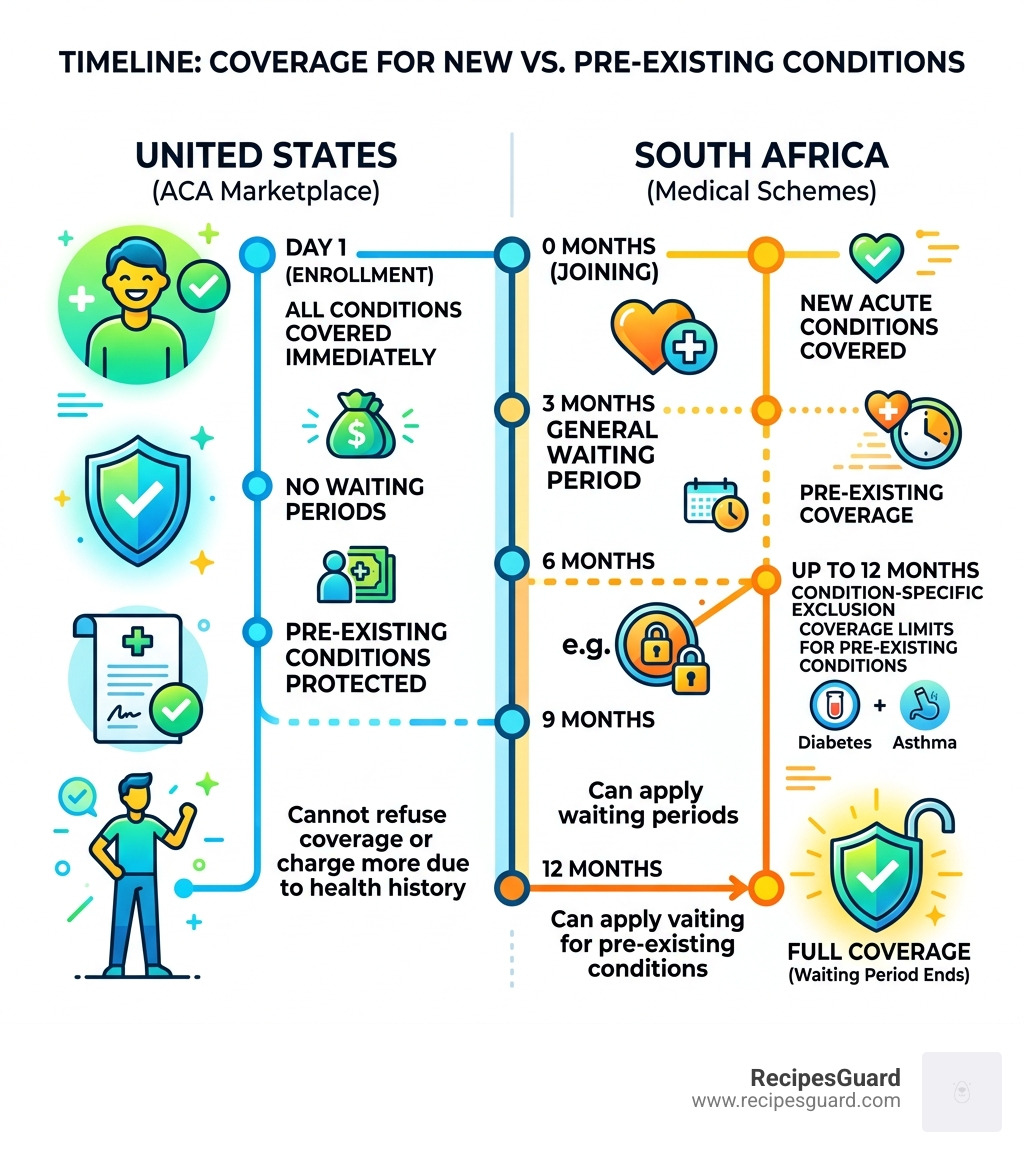
As of April 2026, the core protections put in place by the Affordable Care Act (ACA) in the US still hold — no Marketplace plan can reject you or charge you more because of a pre-existing condition. In South Africa, medical aids operate under different rules, with mandatory waiting periods that can last up to 12 months for certain conditions.
Below, we break down exactly how coverage works, what to watch out for, and how to pick the right plan for your situation.
Learn more about medical aid that covers pre existing conditions:
- family health insurance pre existing condition
- holiday insurance for undiagnosed conditions
Understanding Pre-Existing Conditions and Legal Protections

When we talk about medical aid that covers pre existing conditions, we have to start with the legal backbone of modern health insurance. In the United States, the Affordable Care Act (ACA) changed the game in 2010. Before this, insurance companies could look at your medical history and say, “No thanks,” or charge you a premium that cost more than a small car.
Today, all Marketplace plans are required by law to cover treatment for pre-existing medical conditions. This “no-denial rule” means an insurer cannot reject you, charge you more, or refuse to cover essential health benefits just because you had a condition before your coverage started. For a general overview of how these protections work in the US, see the Affordable Care Act.
Essential Health Benefits and Pregnancy
One of the most important protections involves pregnancy. Under the ACA, pregnancy and childbirth are covered from the very first day your plan starts. You cannot be denied coverage if you are already pregnant when you enroll. Furthermore, giving birth or adopting a child triggers a “Special Enrollment Period,” allowing you to change plans or add your new family member outside of the standard open enrollment dates.
The Exceptions: Grandfathered and Short-Term Plans
While the ACA covers most bases, there are “grandfathered plans”-those that existed before March 23, 2010. These plans aren’t required to follow all ACA rules and might still exclude pre-existing conditions. Similarly, short-term health insurance or “limited benefit” plans often exclude pre-existing conditions entirely. We always recommend checking if a plan is “ACA-compliant” before signing on the dotted line.
Medicaid and the Children’s Health Insurance Program (CHIP) also provide robust protections. They cannot refuse to cover you or charge you higher premiums based on your health status.
Navigating Medical Aid That Covers Pre Existing Conditions in South Africa

In South Africa, the landscape for medical aid that covers pre existing conditions is governed by the Medical Schemes Act. Unlike the US, where coverage is often immediate, South African medical aids use “waiting periods” to protect the pool of funds contributed by all members.
The 12-Month Exclusion and 3-Month Waiting Period
If you join a medical aid in South Africa, you will likely face two types of waiting periods:
- General 3-Month Waiting Period: During this time, you pay your monthly premiums but cannot claim for any benefits except, in some cases, for specific emergency treatments.
- 12-Month Condition-Specific Exclusion: If you have a pre-existing condition (like asthma or diabetes), the scheme can exclude coverage for that specific condition for the first year of your membership.
These rules are not meant to be discriminatory; rather, they prevent people from only joining a medical aid when they are already sick, which would make the system unsustainable for everyone else.
Switching Schemes and Coverage History
If you are moving from one medical aid to another, you might be able to avoid these waiting periods. If you have been a member of a medical scheme for at least two years and switch to a new one within 90 days, the new scheme generally cannot impose a new 12-month exclusion, though they can still apply the 3-month general waiting period. This is why we emphasize the importance of continuous coverage—don’t let your membership lapse!
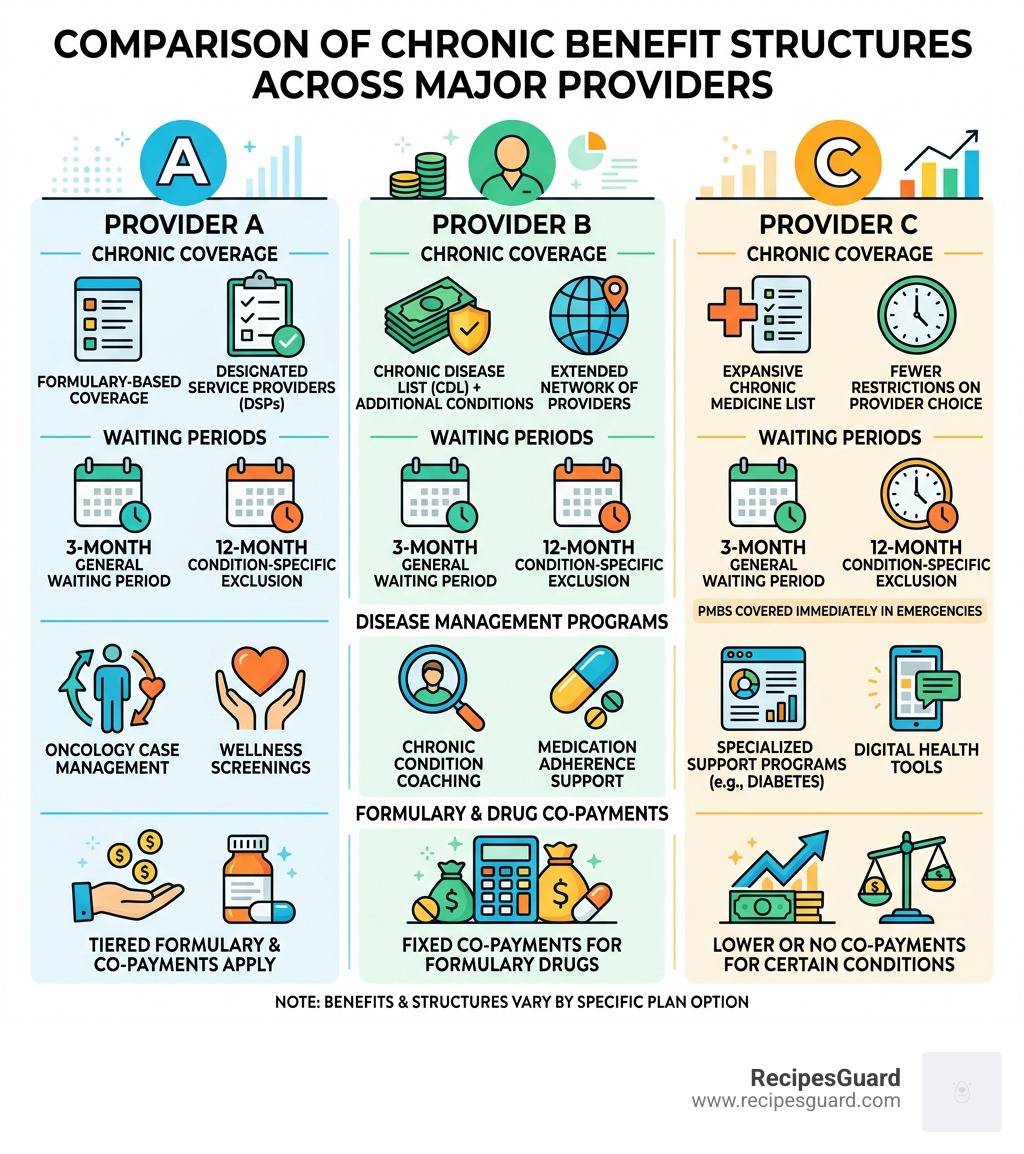
Prescribed Minimum Benefits (PMBs) and Chronic Disease Lists
Even during a waiting period, there is a “safety net” known as Prescribed Minimum Benefits (PMBs). These are a set of defined benefits that ensure all medical scheme members have access to certain minimum health services, regardless of the benefit option they have selected.
The Chronic Disease List (CDL) includes 26 conditions—such as bipolar mood disorder, diabetes, and hypertension—that all medical aids must cover for diagnosis, treatment, and medication.
- Emergency treatment: PMBs cover emergency medical conditions that require immediate treatment.
- Specialized Networks: Many schemes use “Designated Service Providers” (DSPs). If you use a doctor outside of this network for a chronic condition, you might have to pay a co-payment.
- Individualized Treatment Plans: High-end plans often offer clinical case managers who help you manage chronic illnesses through specialized programs.
Travel Insurance and Waivers for Students and Travelers
For our student community traveling abroad, medical aid that covers pre existing conditions often takes the form of travel insurance with a “Pre-existing Condition Waiver.”
The 120-Day Look-Back Period
Most travel insurance providers look at your medical history for the 60 to 120 days before you bought the policy. If you sought treatment, took new medication, or had symptoms of a condition during this “look-back period,” it is considered pre-existing.
Existing Medical Condition Benefit
To get coverage for these issues, you must meet specific requirements for a waiver:
- You must be medically able to travel on the day you buy the plan.
- You must insure the full cost of your trip.
- You usually need to purchase the insurance within a short window (often 14–21 days) of making your initial trip deposit.
This is vital for students who might have managed conditions like Type 2 Diabetes or asthma. With a waiver, your “pre-existing” condition is treated just like any other new illness that might occur during your travels.
Selecting a Medical Aid That Covers Pre Existing Conditions for International Study
When we advise students, we suggest a “health spending audit.” Look back at your last year of medical expenses. How often did you see a specialist? What medications did you refill?
- Provider Network Verification: Ensure the doctors near your university are in the insurance network.
- Specialty Pharmacy Access: If you take biological drugs or rare disease medications, check the “specialty pharmacy” section of the plan.
- Avoiding Gaps: Never let your old insurance end before the new one starts. A gap in coverage can lead to “late joiner penalties” or the loss of “continuous coverage” status.
Essential Tips for Disclosing and Managing Your Coverage
When applying for medical aid that covers pre existing conditions, honesty is the only policy. If you hide a condition, the insurer can reject your claims later, leaving you with massive bills.
| Feature | US ACA Plans | South African Medical Aid |
|---|---|---|
| Can they deny you? | No | No |
| Can they charge more? | No | No (except Late Joiner Penalties) |
| Waiting Periods? | None | 3 to 12 months |
| Exclusions? | None | Specific conditions for 12 months |
Medical Underwriting and Late Joiner Penalties
In South Africa, while they can’t charge you more for being “sick,” they can charge you more for being “late.” If you are over the age of 35 and haven’t had medical aid for a certain period, you may face a Late Joiner Penalty. This is a permanent increase in your monthly premium.
Claim Rejection Risks
Insurers investigate claims by reviewing your medical records. If they find you had a “physiological state” (like pregnancy) or an “acute disease” that you didn’t disclose during underwriting, they can void the policy. We’ve seen cases where undisclosed depression was used to deny physical health claims—don’t take that risk.
How to Choose the Best Medical Aid That Covers Pre Existing Conditions
If you have a chronic condition, a plan with a higher monthly premium but a lower deductible is usually the smarter financial move.
- HSA and FSA: Use Health Savings Accounts to pay for medication with pre-tax dollars.
- Disease Management Programs: Look for plans that offer “Chronic Cover” or specialized oncology benefits. Some comprehensive schemes offer extended oncology benefits once you hit a certain threshold.
- Benefits Investigation: Don’t be afraid to be aggressive. Ask the insurer for a “benefits investigation” to see exactly how much your specific medication will cost under their formulary.
Frequently Asked Questions about Pre-Existing Conditions
Can I be denied health insurance due to a pre-existing condition?
In the US, if the plan is ACA-compliant, no. In South Africa, no, they cannot refuse your membership, but they can make you wait 12 months before they pay for that specific condition.
Is pregnancy considered a pre-existing condition?
Yes, but it is a protected one. In US Marketplace plans, you get day-one coverage. In South Africa, it is subject to the 12-month exclusion, which is why we tell our readers to join a medical aid before planning a family.
How long are the waiting periods for chronic conditions?
Usually, there is a 3-month general waiting period and a 12-month condition-specific exclusion. However, PMBs (Prescribed Minimum Benefits) must be covered from day one in emergencies for South African schemes.
Conclusion
At RecipesGuard, we know that navigating medical aid that covers pre existing conditions can feel like learning a second language. Whether you are a student heading to Australia or someone managing a chronic illness at home, the key is to plan ahead and disclose everything.
We specialize in helping students understand their travel insurance rights and providing step-by-step tutorials on how to file claims so you never get stuck with a bill you can’t pay. Before you pick a plan, do your audit, check the networks, and ensure you have continuous coverage.
Need more help? Check out our guide on selecting the best student health cover.
Final Plan Selection Checklist:
- [ ] Is the plan ACA-compliant (for US) or registered with the CMS (for SA)?
- [ ] Have I disclosed all chronic medications and past surgeries?
- [ ] Are my preferred specialists in the plan’s network?
- [ ] Does the plan offer a Pre-existing Condition Waiver (for travel)?
- [ ] Have I checked the “Chronic Disease List” for my specific condition?

My name is Bianca, and my journey into the world of fermentation and food safety began with a costly mistake. I once lost an entire season’s harvest of chili peppers because I relied on guesswork instead of science. That failure was my turning point.