How to get health insurance when your doctor is still guessing
When Your Body Has Answers but Medicine Doesn’t: Understanding Health Insurance for Undiagnosed Conditions
Health insurance undiagnosed condition coverage is one of the most confusing areas of US health policy — but here’s the short answer:
Under ACA-compliant plans, insurers cannot deny you coverage or charge you more because of a condition, even if it hasn’t been formally diagnosed yet.
Here’s what that means in practice:
- ACA Marketplace plans: Must cover pre-existing and undiagnosed conditions from day one, no waiting periods
- Employer-sponsored plans: Same protections apply under the ACA
- Short-term or grandfathered plans: May still exclude or limit coverage for undiagnosed symptoms — read the fine print carefully
- Undiagnosed ≠ unprotected: Even a symptom you’re still investigating can qualify as a pre-existing condition
Something is clearly wrong. Maybe you’ve had three doctor visits and still no clear diagnosis. Maybe you’re an international student abroad and a confusing medical situation is now colliding with an even more confusing insurance claim.
You’re not alone. Research from community health centers found that over 51% of previously uninsured patients already had at least one pre-existing condition before gaining coverage — and many of those conditions were only formally identified after they got insured. Insurance coverage is often what makes diagnosis possible in the first place.
The system is complex. Insurers deny between 10% and 20% of claims overall, and the reasons are rarely straightforward. For patients with symptoms that don’t yet have a name, the path through coverage, claims, and appeals can feel impossible.
This guide breaks it down clearly — so you know exactly where you stand.
Health insurance undiagnosed condition basics:
- family health insurance pre existing condition
- holiday insurance for undiagnosed conditions
Defining Pre-existing vs. Health Insurance Undiagnosed Condition
When we talk about health insurance, words like “pre-existing” can sound like a legal trap. In the simplest terms, a pre-existing condition is any health issue you had before your new insurance plan started. This includes long-term chronic illnesses like diabetes or high blood pressure, but it also covers temporary injuries or even a surgery you had years ago.
An health insurance undiagnosed condition is slightly different but often treated the same by insurers. This refers to a situation where you are experiencing symptoms—perhaps chronic fatigue, unexplained pain, or neurological “glitches”—but your doctor hasn’t pinned down a name for it yet.
Before the Affordable Care Act (ACA) was passed in 2010, insurance companies could look at these “guessing game” symptoms and decide you were too risky to cover. They could deny your application entirely or charge you “inflated” rates because they suspected a costly diagnosis was around the corner.
Today, Understanding Pre-Existing Conditions Protections means that for most plans, it doesn’t matter if the condition is named or unnamed. You are entitled to coverage. However, the distinction still matters when you are dealing with non-ACA plans or specific travel insurance policies where “honesty is the only policy.”
How Insurers Identify an Undiagnosed Medical Condition
You might wonder, “If I don’t have a diagnosis, how does the insurance company even know something is wrong?” Insurers aren’t mind readers, but they are excellent record keepers. When they determine if a condition is pre-existing (even if undiagnosed), they typically use several tools:
- Look-back Periods: Many plans have a “look-back” window (often 6 to 12 months) where they review your medical activity before the policy started.
- Doctor Notes: They review clinical notes. If you visited a GP three times for “migraines” before your policy began, and later it’s discovered to be a different neurological issue, those initial visits serve as proof that the condition existed.
- Prescription History: Even without a diagnosis, if you were prescribed medication to manage symptoms (like an inhaler for “shortness of breath”), that is a paper trail.
- Symptom Onset: If you suddenly claim for a major surgery two days after a policy starts, insurers will look for “objective evidence” that you were seeking help for those symptoms previously.
- Diagnostic Codes: Every time a doctor bills insurance, they use ICD-10 codes. Even if the code is just for “unspecified abdominal pain,” it marks the start of that medical history.
ACA Protections and Plan Types That Cover the Unknown
Navigating the insurance market in April 2026 feels like walking through a maze. The most important thing we tell students and families is that not all plans are created equal.
If you have an health insurance undiagnosed condition, your best bet is an ACA-compliant plan. These plans are legally required to cover you regardless of your health status. On the other hand, “short-term” plans or “limited benefit” plans often operate under the old rules, where they can exclude anything they deem pre-existing.
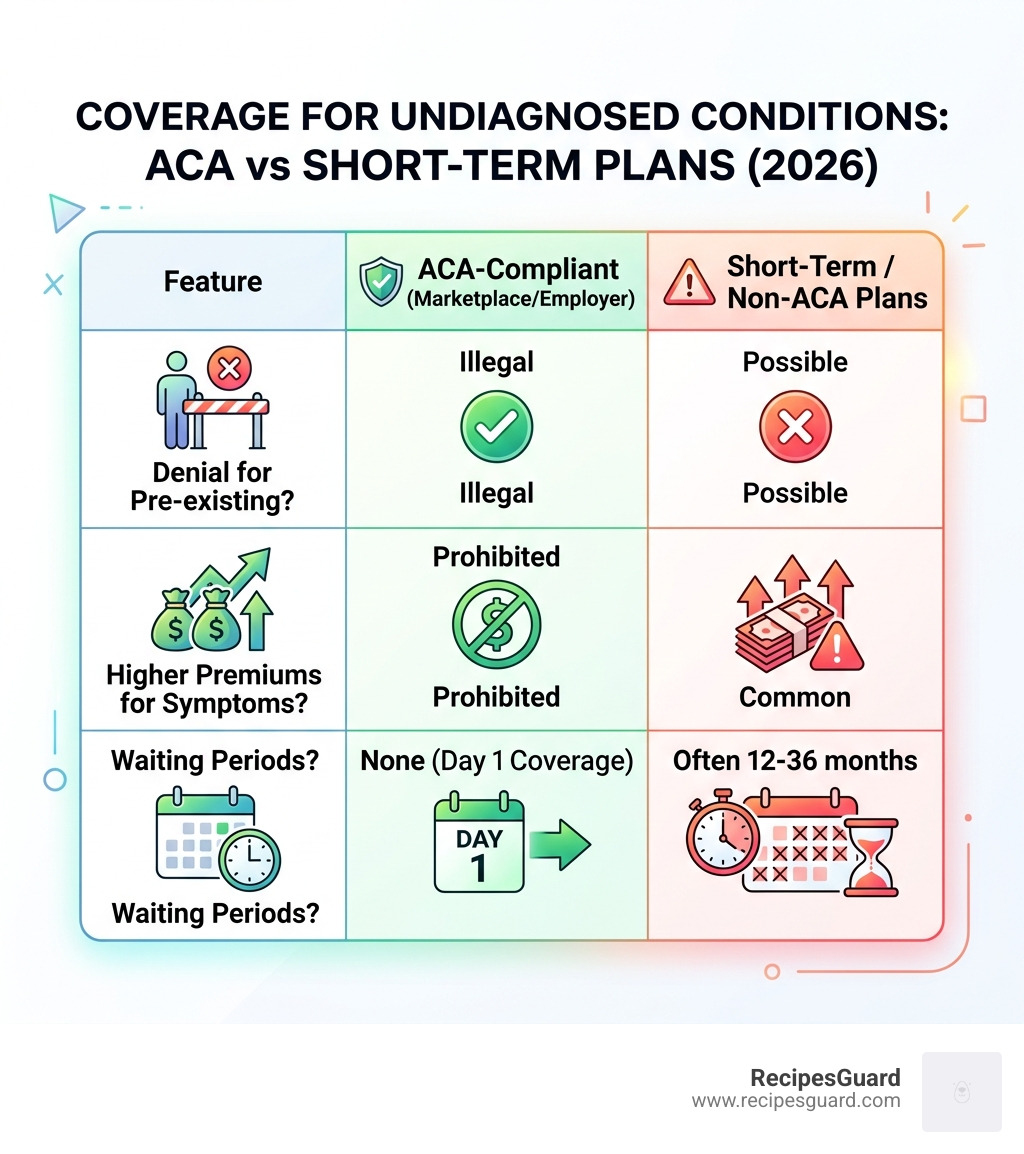
| Feature | ACA-Compliant (Marketplace/Employer) | Short-Term / Non-ACA Plans |
|---|---|---|
| Denial for Pre-existing? | Illegal | Possible |
| Higher Premiums for Symptoms? | Prohibited | Common |
| Waiting Periods? | None (Day 1 Coverage) | Often 12-36 months |
| Covers Undiagnosed Symptoms? | Yes | Usually Excluded |
| Essential Health Benefits? | Guaranteed | Not Guaranteed |
Under Coverage for Pre-existing Conditions, Marketplace plans and most job-based plans must cover treatment for your condition right away. This is vital because, as research shows, many people only get their symptoms diagnosed because they finally gained access to the specialists and testing that insurance provides.
Special Considerations for a Health Insurance Undiagnosed Condition
Certain life events and conditions have unique protections or challenges:
- Pregnancy: This is considered a pre-existing condition, but under the ACA, you cannot be denied coverage or charged more if you are already pregnant when you sign up. Coverage for the pregnancy and delivery begins the day your plan starts.
- Mental Health: Anxiety, depression, and substance misuse are often the most common “undiagnosed” issues. Post-ACA data shows that mental health diagnoses surged by nearly 18% among those who gained insurance, proving that coverage is the key to identifying these needs.
- Rare Diseases: If you are in the “diagnostic odyssey”—searching for a name for a rare genetic disorder—genetic testing is a major hurdle. Some plans require heavy prior authorization for these expensive tests.
- Chronic Pain: Symptoms like undiagnosed leg pain or nerve damage are common. While covered by ACA plans, they are often the target of “medical necessity” reviews, which we will discuss below.
Why Claims for Undiagnosed Symptoms Get Denied

It’s a gut-punching moment: you finally get the test your doctor ordered, but the insurance company sends a letter saying they won’t pay. Even though the law protects your right to get insurance, it doesn’t always stop insurers from questioning individual claims.
According to How Often Do Health Insurers Deny Patients’ Claims? — ProPublica, health insurers deny between 10% and 20% of the claims they receive. Shockingly, some Marketplace plans have been found to deny as many as 1 in 3 claims.
Common reasons for denial when dealing with an health insurance undiagnosed condition include:
- Lack of Medical Necessity: The insurer argues that the test (like an expensive MRI) isn’t “necessary” because there isn’t a confirmed diagnosis yet.
- Prior Authorization Failures: Your doctor didn’t get the “okay” from the insurer before performing the service.
- Administrative Errors: Simple things like a misspelled name or an incorrect insurance ID number.
- Coordination of Benefits (COB): The insurer thinks you have another primary insurance plan and refuses to pay until you prove otherwise.
Navigating a Health Insurance Undiagnosed Condition Claim
When your claim is “pending,” it usually means the insurer is waiting for more information. This is common for undiagnosed symptoms because the insurer wants to see the doctor’s “clinical notes” to justify the cost.
To keep your claim moving:
- Check the ICD-10 and CPT Codes: The ICD-10 code is your diagnosis (or symptom), and the CPT code is the procedure. If these don’t “match” in the insurer’s computer system, the claim will kick back.
- Ask for the “Member Impact”: Is the denial based on a paperwork error, or are they saying the service isn’t covered by your policy?
- Monitor the “Float” Time: Sometimes a claim is approved, but the payment takes 2-3 weeks to reach your doctor. Don’t panic and pay the full bill out of pocket until you see your final Explanation of Benefits (EOB).
Steps to Take if Your Claim is Rejected
If you receive a denial, don’t give up. Research shows that less than 1% of people appeal their denials, yet those who do often see results. Insurers sometimes count on patients being too tired or sick to fight back.
- Get it in Writing: You need a formal letter stating exactly why the claim was denied.
- Internal Appeal: Ask your insurer to reconsider. This is where your doctor’s clinical notes are your best weapon. They must explain why the “guessing” phase required specific tests.
- External Review: If the internal appeal fails, you can take it to an independent third party. This is a powerful tool under the ACA.
- Contact Your State Insurance Department: They oversee how insurers behave in your state and can intervene if a company is acting unfairly.
- Seek Financial Assistance: Many hospitals have “charity care” or financial assistance programs for patients facing high costs for undiagnosed or rare conditions.
As noted in the NBC News investigates insurance denials report, systemic issues like prior authorization are making denials more frequent. We have seen cases where media or regulatory intervention was the only thing that moved a stagnant claim.
Frequently Asked Questions about Undiagnosed Conditions
Can I be denied coverage for a symptom that hasn’t been named yet?
If you are applying for an ACA-compliant plan (Marketplace or Employer-based), the answer is a firm no. They cannot deny you coverage or charge you more just because you are experiencing symptoms that haven’t been diagnosed. However, if you are looking at short-term or “grandfathered” plans, they can—and likely will—deny coverage for those symptoms.
Do grandfathered plans have to cover my undiagnosed symptoms?
Not necessarily. “Grandfathered” plans are those that existed before the ACA was signed in March 2010 and haven’t changed significantly since. These plans are exempt from many ACA protections, meaning they can still exclude pre-existing conditions or charge higher rates. If you’re on one of these, it might be time to look for a Marketplace alternative.
How do I prove a condition wasn’t pre-existing?
This usually comes up with travel insurance or non-ACA plans. You’ll need your medical records to show that you never sought treatment, took medication, or mentioned the specific symptoms to a doctor before the policy’s effective date. If your tests and scans were negative in the past and you were symptom-free, you generally don’t have to declare it as a “condition.”
Conclusion
Navigating the medical system is exhausting enough when you’re feeling well; it’s a marathon when you’re sick and your doctor is still looking for answers. But remember: health insurance undiagnosed condition protections are there to ensure that the “guessing” phase doesn’t bankrupt you.
At RecipesGuard, we specialize in helping students navigate these exact hurdles. Whether you’re an international student trying to understand a US “Explanation of Benefits” or a family dealing with a sudden medical mystery, we believe transparency is the best medicine.
Don’t let a “Pending” status or a “Denied” stamp be the final word on your health. Stay persistent, use your right to appeal, and always choose ACA-compliant coverage when possible to protect your future.

My name is Bianca, and my journey into the world of fermentation and food safety began with a costly mistake. I once lost an entire season’s harvest of chili peppers because I relied on guesswork instead of science. That failure was my turning point.
