Steps to Submit Medical Expense Claims Without Losing Your Mind
Why Every Patient Needs a Medical Bill Dispute Guide in 2026
A medical bill dispute guide can save you hundreds — sometimes thousands — of dollars. Medical bills are confusing by design, and errors are shockingly common. Here is what you need to know right now:
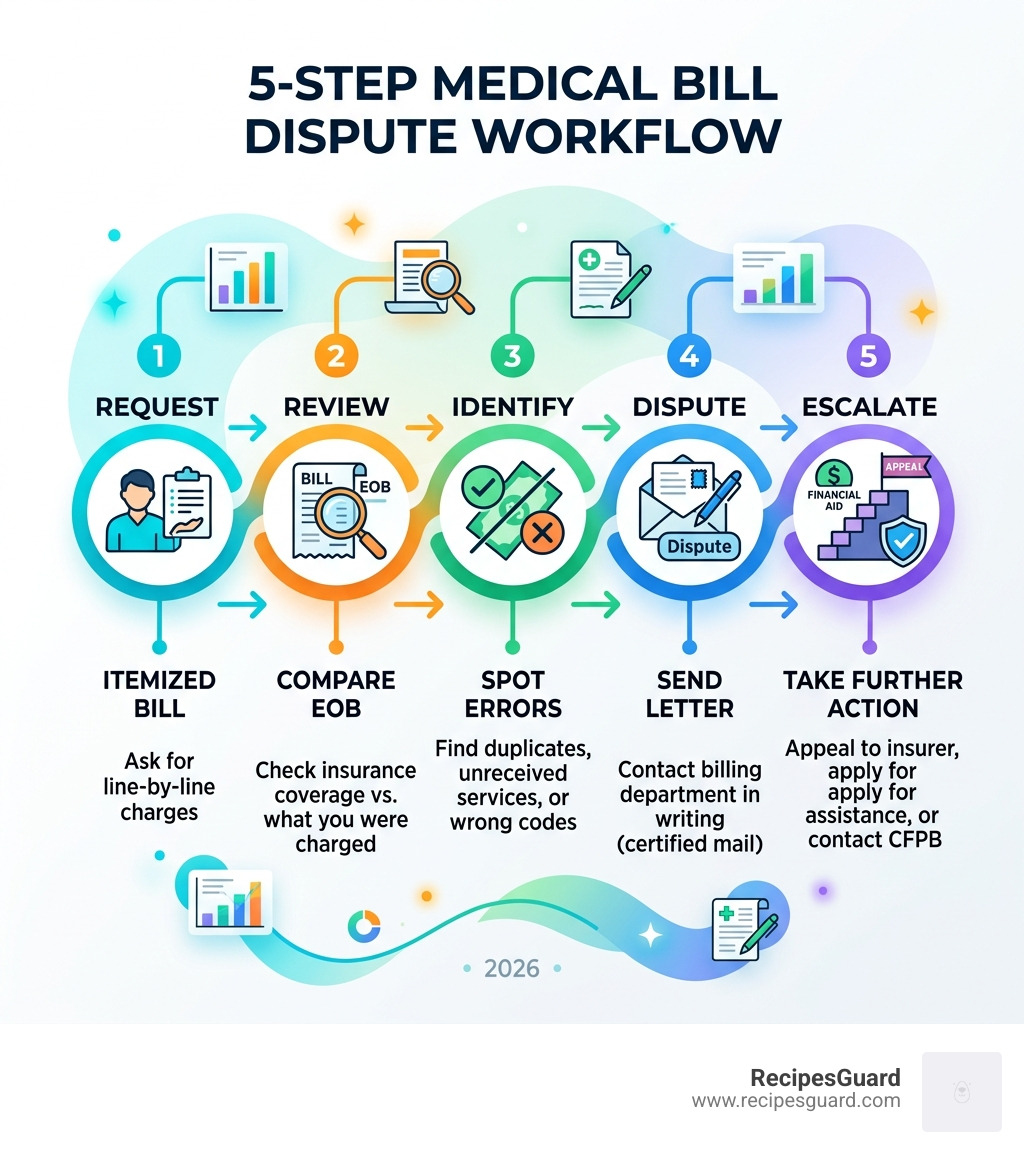
Quick Steps to Dispute a Medical Bill:
- Request an itemized bill — ask for every charge broken down line by line
- Compare it to your Explanation of Benefits (EOB) — spot what insurance covered vs. what you were charged
- Identify errors — look for duplicate charges, services never received, or wrong codes
- Contact the billing department in writing — send a dispute letter by certified mail with a 30-day response deadline
- Escalate if needed — appeal to your insurer, apply for financial assistance, or contact the CFPB
Medical debt is one of the biggest financial stressors in the US right now. As of 2021, there was $88 billion in medical bills sitting on consumer credit reports — showing up on 43 million people’s files. About one in five households carries unpaid medical bills.
If you are an international student dealing with a medical bill from a foreign healthcare system, the confusion is even worse. You may not know your rights. You may not know which charges are legitimate. You may feel pressured to just pay and move on.
Don’t.
The good news? 78% of people who disputed an incorrect medical bill resolved it in their favor. That number comes from a 2024 survey of North Carolina residents — and it shows that pushing back works.
The bad news? It takes persistence. On average, professional case managers make 22 phone calls to fully resolve a medical billing case. That is a lot — but knowing the process makes it far less overwhelming.
This guide walks you through every step, from spotting errors to protecting your credit.
Medical bill dispute guide terms you need:
Identifying Errors: Your Medical Bill Dispute Guide to Accuracy
When that “Summary of Charges” arrives in the mail, it often looks like a single, terrifying number. But that summary is just the tip of the iceberg. To truly understand what you are being charged for, you must go deeper. Industry experts suggest that up to 80% of medical bills contain at least one error. This is why a medical bill dispute guide is your best friend when navigating the healthcare system.
The first rule of medical billing: Never pay the first bill you receive. Instead, your very first move should be to get paid back for your doctor visits by ensuring the numbers are actually correct.

Common Red Flags in Hospital Billing
Errors aren’t always malicious; often, they are the result of a busy hospital staff entering data into a complex system. However, these “data entry” mistakes can cost you thousands. Here are the red flags we look for:
- Upcoding: This is when a provider bills for a more expensive service than what was actually performed. For example, a routine 15-minute office visit might be billed as a complex 45-minute consultation.
- Duplicate Billing: It is incredibly common to see the same procedure, medication, or lab test listed twice on the same day.
- Unbundling: Some procedures are meant to be billed as a single “package” or bundle. Unbundling happens when a provider lists every single component of that procedure separately to increase the total cost.
- Balance Billing: This occurs when a provider bills you for the difference between their “sticker price” and what your insurance agreed to pay. In many cases, especially under the No Surprises Act, this is illegal.
- Services Not Rendered: You might find charges for a specialist you never saw or a medication you refused while in the hospital. Always check for “phantom services.”
If you spot these, don’t panic. You just need to know what to do if your medical bill has mistakes to get them cleared.
Using the EOB as a Medical Bill Dispute Guide
Before you even talk to the hospital, you need to look at your Explanation of Benefits (EOB). Your EOB is not a bill; it is a document from your insurance company explaining what they paid and what they didn’t.
Compare the itemized bill from the hospital with the EOB. If the hospital is asking for $500, but the EOB says your “Patient Responsibility” is only $150, the hospital has likely made a billing error or is attempting to balance bill you. If a claim was denied, the EOB will provide a reason code. Understanding these codes is the secret to claiming medical expenses without the headache.
Navigating the No Surprises Act and Federal Protections
As we move through 2026, the No Surprises Act remains the most powerful shield for patients. This federal law was designed to stop “surprise” bills—those moments when you go to an in-network hospital but are treated by an out-of-network doctor (like a radiologist or anesthesiologist) who then sends you a massive bill.
The Act covers:
- Emergency services at out-of-network facilities.
- Non-emergency services provided by out-of-network doctors at in-network hospitals or surgical centers.
- Air ambulance services (though ground ambulances are often still a gray area).
For students and travelers, understanding how to handle the hospital stay claim process under these protections is vital to avoiding financial ruin.
Qualifications for the Patient-Provider Dispute Resolution (PPDR)
If you are uninsured or choose to “self-pay” (not use your insurance), you have specific rights under the PPDR process. When you schedule a service at least three days in advance, the provider must give you a Good Faith Estimate (GFE).
You qualify to use the official CMS dispute process if:
- You did not use insurance for the service.
- You received a GFE before the service.
- The final bill is at least $400 higher than the GFE.
- You file the dispute within 120 calendar days of receiving the bill.
There is a $25 administrative fee to start this process, but if you win, that amount is usually deducted from what you owe. This is a formal way to dispute a medical bill via CMS.
Protecting Your Rights Under the No Surprises Act
Providers are now required to be transparent about their network status. If you are at an in-network facility, you should not be charged out-of-network rates for ancillary services. If you receive a bill that seems to violate these rules, you can file a complaint at the CMS No Surprises Help Desk.
Knowing how to dispute a surprise medical bill is about more than just saving money; it’s about holding the healthcare system accountable to the law.
Step-by-Step: How to Dispute a Medical Bill Successfully
Disputing a bill is a marathon, not a sprint. Statistic about the 22 phone calls? That’s not a joke. To stay sane, you need a system.
Organizing Your Medical Bill Dispute Guide Documentation
The person who wins a billing dispute is usually the one with the best records. We recommend keeping a “Dispute Folder” (digital or physical) that includes:
- Call Logs: Every time you call, write down the date, the time, the name of the person you spoke to, their employee ID (if they’ll give it), and exactly what was promised.
- Itemized Statements: Keep every version of the bill you receive.
- Insurance Policy: Have your policy numbers and medical reports paperwork trail ready.
- Certified Mail Receipts: If you send a dispute letter, send it via certified mail with a return receipt. This proves they received it and starts the clock on their 30-day response window.
Following the steps in mastering the student medical claim process will keep your documentation airtight.
Communicating with Providers and Insurers
When you call the billing department, stay calm but firm. Use the “three-way call” tactic: if the hospital says the insurance didn’t pay, and the insurance says the hospital billed incorrectly, get them both on the line together. It is much harder for them to point fingers when they are talking to each other.
If the first-level representative can’t help you, politely ask to speak with a billing supervisor. Persistence is key. As noted in research on how to dispute a medical bill, being polite and organized often yields better results than getting angry.
Negotiating Discounts and Financial Assistance Programs
What if the bill is technically “correct,” but you simply cannot afford to pay it? This is where negotiation and financial assistance (often called “Charity Care”) come into play.
| Program Type | Best For | Typical Benefit |
|---|---|---|
| Charity Care | Low-to-mid income patients | 50% to 100% bill forgiveness |
| Lump Sum Discount | Patients with some savings | 10% to 40% off for immediate payment |
| Payment Plans | Most patients | 0% interest monthly installments |
| Medical Advocate | Complex, high-dollar cases | Professional dispute resolution (contingency fee) |
Using these tools makes claiming medical expenses as a student much more manageable.
How to Apply for Hospital Charity Care
Many people don’t realize that non-profit hospitals are required by law to have financial assistance programs. These aren’t just for the very poor; many hospitals offer discounts to families earning up to 400% of the Federal Poverty Level.
To apply, you will typically need to provide:
- Recent tax returns or pay stubs.
- Bank statements.
- A written explanation of your financial hardship.
Be mindful of deadlines! Some hospitals require you to apply for assistance within 45 days of being discharged.
Negotiation Tactics for Lower Payments
If you don’t qualify for charity care, you can still negotiate. Hospitals would rather get some money than no money.
- The “Medicare Rate” Strategy: Ask the hospital what Medicare pays for the same service. Offer to pay that amount (which is usually much lower than the “chargemaster” price).
- Prompt-Pay Discount: Ask if they offer a discount for paying the full (negotiated) balance immediately.
- Hardship Letters: If you are a student, write a letter explaining your situation. Mention that you are an international student with limited funds.
If the bill is over $10,000 and you are overwhelmed, consider hiring a medical billing advocate. They usually work on contingency, meaning they only get paid if they save you money.
Protecting Your Credit and Handling Collections
One of the biggest fears with medical bills is the impact on your credit score. Fortunately, the rules have changed in favor of the consumer.
Your Rights During the Dispute Process
Under the Fair Debt Collection Practices Act (FDCPA), you have rights. If a bill is sent to collections while you are actively disputing it:
- Send a Validation Letter: You have 30 days from the first contact to demand that the collector “validate” the debt. They must prove the debt is yours and the amount is correct.
- Collection Pause: Once you dispute the debt in writing, the collector must stop trying to collect until they provide the validation.
- Credit Reporting Thresholds: As of 2023, medical bills under $500 should not appear on your credit report at all. Furthermore, paid medical debts are removed from credit reports, and unpaid ones can only be reported after a 12-month waiting period.
Whether you are in the US or learning how to handle medical bills down under, these credit protections are your safety net.
What to Do if a Resolved Bill Persists
Sometimes, even after you win a dispute, the “system” doesn’t update, and you keep getting bills. If this happens:
- Send a final “Settlement Letter” via certified mail showing the dispute resolution.
- If they continue to harass you, file a complaint with the Consumer Financial Protection Bureau (CFPB).
- For No Surprises Act violations, contact the federal help desk immediately.
Frequently Asked Questions about Medical Bill Disputes
How long do I have to dispute a bill before it goes to collections?
Typically, you have a 60-to-90-day window from the first billing statement before a provider sends the account to a collection agency. However, if you are in active communication with the billing department, they will often “hold” the account. Always ask them to put a “billing hold” on your account while the dispute is under review.
What if my insurance company denies a claim for a necessary service?
You have the right to an internal appeal. Ask your doctor to write a “Letter of Medical Necessity” explaining why the service was required. If the internal appeal fails, you can request an external review by an independent third party.
When should I hire a professional medical billing advocate?
Consider an advocate if:
- The bill is over $5,000.
- You have had multiple surgeries with dozens of separate bills.
- You have been denied through two rounds of insurance appeals.
- You are physically or mentally unable to handle the “22 calls” required for resolution.
Conclusion
Navigating medical billing is undeniably stressful, especially for students and travelers far from home. However, you are not powerless. By using this medical bill dispute guide, staying organized, and being persistent, you can protect your financial health.
The system is complex, but it is also full of errors that can be corrected. Don’t let a “phantom charge” or a “surprise bill” ruin your credit or your peace of mind. Stand your ground, ask for the itemized breakdown, and don’t be afraid to escalate your concerns to the proper authorities.
At RecipesGuard, we are dedicated to helping students navigate these complex insurance and medical landscapes. Your focus should be on your studies and your health — not on fighting an incorrect invoice. For more step-by-step tutorials on handling claims and protecting your rights abroad, visit our main site at https://www.recipesguard.com/.

My name is Bianca, and my journey into the world of fermentation and food safety began with a costly mistake. I once lost an entire season’s harvest of chili peppers because I relied on guesswork instead of science. That failure was my turning point.