Don’t Let Your Medical History Stop Your Future Disability Coverage
Your Medical History Doesn’t Have to Block Your Disability Coverage
Disability insurance that covers pre-existing conditions is more available than most people think — and finding the right path starts with knowing your options.
Here’s a quick answer if you’re short on time:
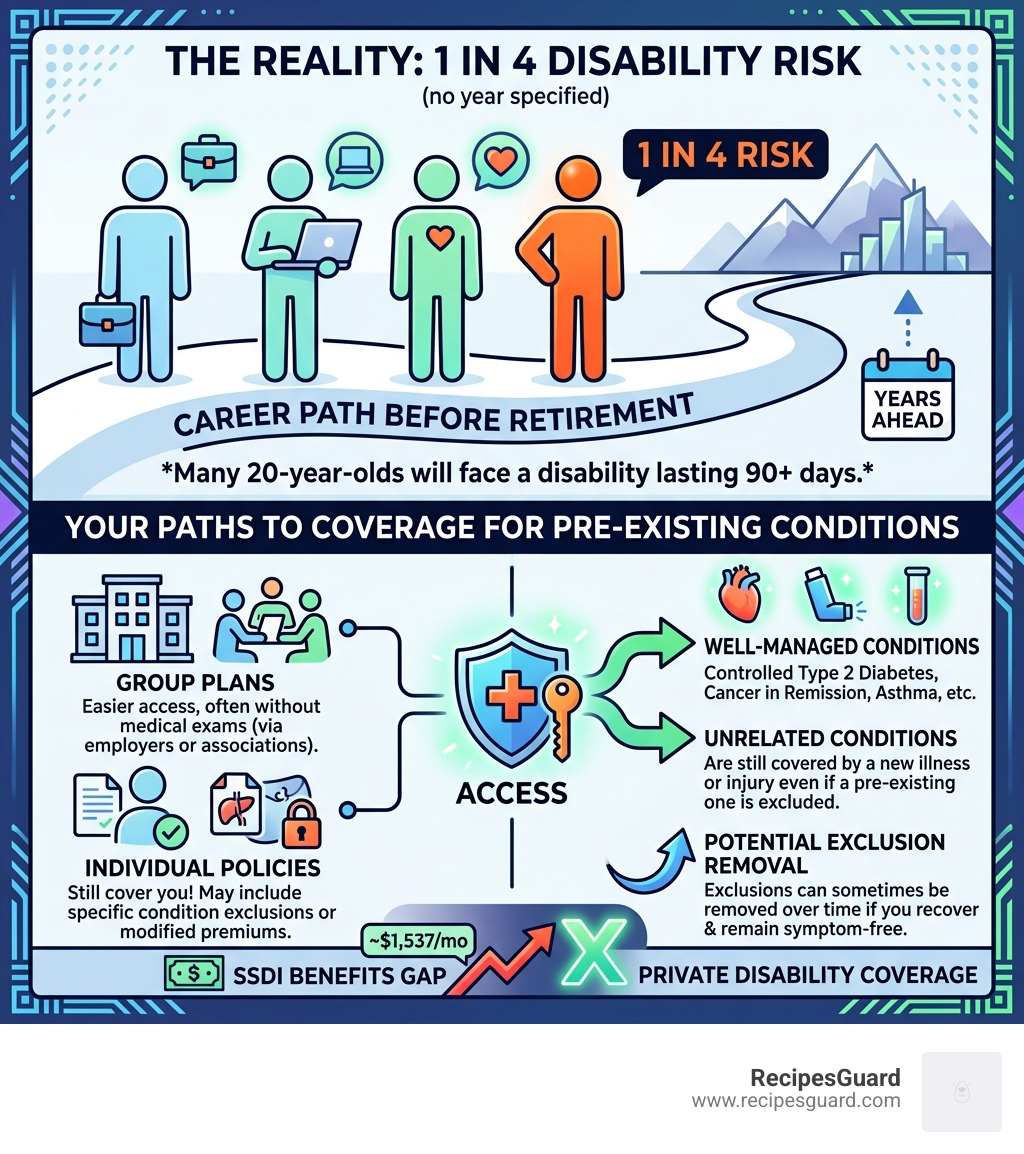
- Group plans (through employers or professional associations) often don’t require a medical exam and offer the easiest access for people with health history
- Individual policies can still cover you — often with an exclusion rider for the specific condition, or a slightly higher premium
- Well-managed conditions like Type 2 diabetes, cancer in remission, or controlled asthma may qualify for standard or modified coverage
- Unrelated conditions are still covered — even if your pre-existing condition is excluded, a new illness or injury is typically covered
- Some exclusions can be removed over time if you recover and remain symptom-free
The stakes are real. One in four 20-year-olds will experience a disability lasting 90 days or more before retirement age. And if you’re studying or working abroad, losing your income without a safety net can be devastating fast.
The average Social Security Disability Insurance (SSDI) benefit pays only around $1,537 per month — and only 38% of applicants are even approved on their first try. Private disability coverage fills that gap.
The good news? A pre-existing condition is not an automatic door slam. It changes how you get covered, not always whether you get covered.
Disability insurance that covers pre existing conditions terms at a glance:
- family health insurance pre existing condition
- holiday insurance for undiagnosed conditions
Defining Pre-Existing Conditions and Underwriting Realities
When we talk about disability insurance that covers pre-existing conditions, we first need to understand what insurers are looking for. In the insurance world, a pre-existing condition is generally any illness, injury, or medical condition you were diagnosed with or treated for before applying for coverage. This can range from chronic issues like asthma or diabetes to past surgeries or even mental health history like anxiety and depression.
The process of evaluating your health is called medical underwriting. During this phase, the insurer reviews your medical records, looking at the diagnosis, the severity of the condition, and how stable your treatment has been. They aren’t just looking for “perfect” health; they are assessing the statistical likelihood that your condition will prevent you from working in the future.
For many of us, especially students or young professionals in Australia, this can feel like a daunting “background check.” However, insurers often distinguish between minor illnesses (like a past flu) and chronic conditions. To get a better grasp of this process, you can explore Understanding Medical Underwriting for Disability Coverage | RecipesGuard Resources. By being transparent about your medical history from the start, you actually reduce the risk of a claim being denied later due to non-disclosure.
Can You Get Disability Insurance That Covers Pre-Existing Conditions?
The short answer is yes, but it often comes with “modifications.” Insurers have a few tools they use to manage the risk of a pre-existing condition. If you have a well-managed condition, you might still get a policy, but the insurer may add an exclusion rider. This means the policy will cover you for any new injury or illness, but it won’t pay out if you become disabled specifically because of that pre-existing condition.
For example, if you have a history of chronic back pain, the insurer might exclude “spinal disorders.” If you break your leg or develop a different illness, you’re fully covered. But if your back flares up and keeps you from work, that specific claim would be denied.
Another option is a premium rating. Instead of excluding the condition, the insurer might agree to cover it but charge a higher premium—sometimes 25% to 50% more—to account for the extra risk.
| Feature | Exclusion Rider | Premium Rating |
|---|---|---|
| Coverage for Pre-existing Condition | No | Yes |
| Premium Cost | Standard | Higher |
| Coverage for New Injuries | Yes | Yes |
| Best For | Specific, isolated injuries | Chronic, well-managed health issues |
Qualifying for Disability Insurance That Covers Pre-Existing Conditions via Group Plans
For many students and employees, group disability plans are the “golden ticket.” These are often offered through an employer or a professional association. The biggest advantage? They often feature guaranteed issue coverage. This means you can get a base level of protection without undergoing a medical exam or answering detailed health questions.
In Australia, many superannuation funds include Total and Permanent Disability (TPD) insurance as a default. While these group plans are easier to join, they often have “pre-existing condition exclusion” clauses that apply for a set period (usually the first 12 to 24 months of the policy). If you stay healthy and work through that window, the condition might eventually be covered.
How Individual Disability Insurance That Covers Pre-Existing Conditions Handles Underwriting
If you want more robust protection—like “own-occupation” coverage that pays out if you can’t perform your specific job—you’ll likely need an individual policy. This involves full medical underwriting.
While this sounds strict, it allows for more personalization. We recommend being completely honest during this process. If you hide a condition and the insurer finds out during the “contestability period” (usually the first two years), they can cancel your entire policy. For a deeper dive into these options, check out our Comprehensive Guide to Individual Disability Income Protection.
Understanding the Lookback Period and Safe Harbor Rules
When an insurer looks at a claim, they often use a lookback period. This is a specific window of time (typically 3 to 12 months) before your coverage started. They check your medical records to see if you received treatment or showed symptoms for your current disability during that time.
If you are covered under a group plan, you might benefit from the 12-month safe harbor rule. This rule generally states that if you work continuously for 12 months after your coverage begins without a disability claim, the pre-existing condition exclusion expires. After that year is up, your pre-existing condition is often treated just like any other illness.
Critical Time Periods to Remember:
- Lookback Period: The 3–6 months before your policy starts where insurers check for symptoms.
- Filing Window: The first 12–24 months of a policy where pre-existing exclusions are most strictly enforced.
- Elimination Period: The “waiting period” (often 90 days) between becoming disabled and receiving your first check.
- Contestability Period: The first 2 years where an insurer can cancel a policy for application mistakes.
How to Challenge a Claim Denial Based on Medical History

It is a frustrating reality: insurance companies sometimes deny claims by stretching the definition of a pre-existing condition. They might try to link a new disability to an unrelated symptom from years ago. For instance, they might claim a stroke was “pre-existing” because you were treated for high blood pressure. Legally, however, treating a risk factor is not the same as being treated for the disabling condition.
If your claim is denied, don’t take it at face value. Many denials are based on “but-for” causation, which is often legally insufficient. Courts generally require proximate causation, meaning the pre-existing condition must be the direct and primary cause of the disability.
To fight back, you should:
- Request a clear reason: Insurers are legally required to explain the denial in writing.
- Get a physician’s statement: Ask your doctor to write a letter explaining the medical distinction between your past history and your current disability.
- Review the language: If the policy language is ambiguous (e.g., what counts as “treatment”), Australian law typically favors the policyholder.
For more help on this, see our guide on Navigating Pre-existing Condition Exclusion Clauses in Claims.
Frequently Asked Questions about Disability Insurance and Health History
Does the Affordable Care Act (ACA) affect disability insurance pre-existing conditions?
One of the biggest misconceptions we see is that the ACA (Obamacare) protects disability insurance applicants. It does not. The ACA’s rules against denying coverage for pre-existing conditions apply only to health insurance. Disability insurers are still allowed to use medical underwriting, exclude conditions, or deny applications based on your health history.
Can an insurer deny a claim for a condition I didn’t know I had?
Generally, no. The “reasonable person” standard usually applies. An insurer shouldn’t deny a claim for a condition that was undiagnosed and didn’t present symptoms that would cause a reasonable person to seek medical attention. If you had a routine screening (like a mammogram) that came back clear, that is considered “diagnostic,” not “treatment” for a pre-existing condition.
Are pre-existing condition exclusions permanent?
Not always! This is great news for those who have recovered from past injuries. If you have been symptom-free and haven’t required treatment for a specific period (often several years), you can sometimes ask the insurer to review and remove an exclusion rider. For example, if you had a back injury five years ago but have had no issues since, an insurer might agree to cover your back fully after a new medical review.
Conclusion
Securing disability insurance that covers pre-existing conditions is a vital part of financial planning in 2026. Whether you are a student in Australia or a professional mid-career, your ability to earn an income is your most valuable asset. While a medical history can add a few hurdles to the application process, it is rarely a total roadblock.
At RecipesGuard, we specialize in helping students and young professionals navigate the complexities of insurance. From step-by-step claim filing tutorials to advisory services, we ensure you don’t have to face the insurance giants alone. If you’re ready to protect your future, you can find more info about RecipesGuard services on our website. Don’t wait until an illness occurs to look for a safety net—start your planning today.

My name is Bianca, and my journey into the world of fermentation and food safety began with a costly mistake. I once lost an entire season’s harvest of chili peppers because I relied on guesswork instead of science. That failure was my turning point.
