What You Need to Know About the Hospital Stay Claim Process
The hospital stay claim process can feel overwhelming — especially if you’ve never dealt with a medical bill or insurance form before. Whether you are an international student in Australia or navigating the system in the US, a surprise hospitalization is stressful enough on its own. Add in unfamiliar paperwork, tight deadlines, and confusing insurance jargon, and it’s easy to feel lost.
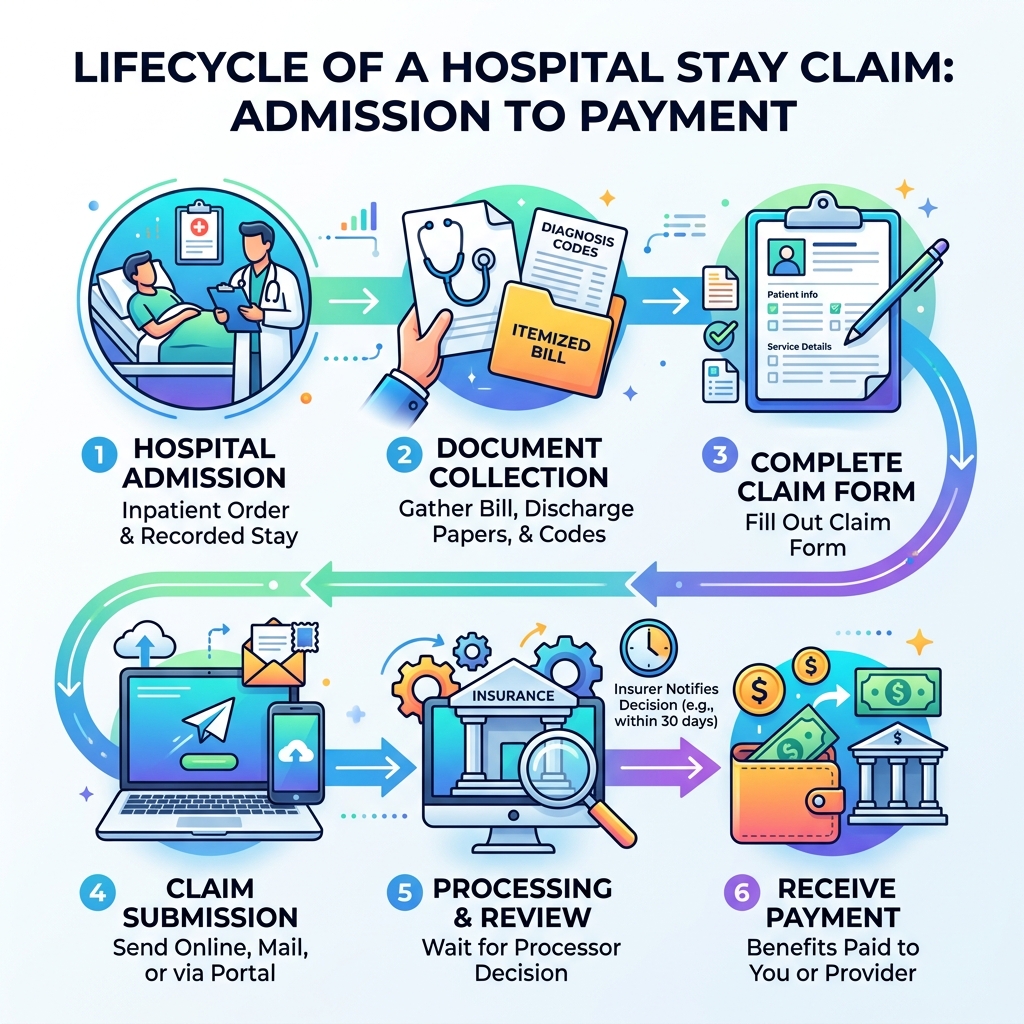
Here’s a quick overview of how the process works:
- Get admitted – Your doctor issues a formal inpatient order and the hospital records your stay.
- Collect your documents – Gather your itemized hospital bill, discharge papers, diagnosis codes, and proof of payment.
- Complete your claim form – Fill out your insurer’s claim form (or the Medicare CMS-1490S form if applicable).
- Submit your claim – Send it online, by mail, or through your insurer’s member portal — with all supporting documents attached.
- Wait for processing – Insurers are typically required to notify you of a decision within 30 business days.
- Receive payment – Benefits are paid directly to you or your provider, depending on your plan.
- Appeal if denied – If your claim is rejected, you have the right to file a formal appeal.
Nearly 34 million people are admitted to a hospital every year in the US, and over 11 million in Australia. And the average cost of just a three-day stay runs around $30,000 in some regions. For international students or anyone without solid coverage, that kind of bill can be financially devastating.
The good news? Once you understand the steps, the process is manageable — even if it’s your first time.
Understanding Hospital Indemnity vs. Traditional Health Insurance
When we talk about the hospital stay claim process, it is vital to distinguish between major medical insurance and hospital indemnity insurance. Whether you are an international student in Australia or the US, think of major medical as your “base layer”—it pays the doctors and the facility for the actual cost of care. Hospital indemnity, on the other hand, is like a financial safety net designed to catch the costs that fall through the cracks.
What Is Hospital Indemnity Insurance? It is a supplemental policy that provides fixed cash benefits. Unlike traditional health insurance, which pays a percentage of your bill, indemnity plans pay a set amount per day or per event, regardless of what the hospital actually charges you.
Statistics show that The average cost of a three-day hospital stay is around $30,000. With millions of admissions annually across the US and Australia, many patients find themselves facing high out-of-pocket costs even with “good” insurance. Deductibles, co-pays, and non-medical expenses like travel or lost wages can quickly add up.

| Feature | Major Medical Insurance | Hospital Indemnity Insurance |
|---|---|---|
| Who it pays | Usually the doctor or hospital | Usually YOU (the policyholder) |
| Payment Amount | Based on actual medical costs | Fixed daily or per-event rate |
| Usage | Restricted to medical bills | Flexible (rent, groceries, etc.) |
| Network | Often requires “in-network” care | Generally works with any hospital |
Eligibility and Coverage Scope
Most of us can secure this coverage through an employer, often via simple payroll deduction. One of the best parts about indemnity plans is the family coverage options. You can typically include a spouse and dependent children (often up to age 26).
The scope of coverage is surprisingly broad. While it focuses on inpatient stays, many policies also trigger payments for:
- Intensive Care Unit (ICU) stays (often at a higher daily rate).
- Ambulance rides (ground or air).
- Emergency room visits.
- Outpatient surgeries.
Importantly, these plans are generally HSA-compatible, meaning you can have a High Deductible Health Plan (HDHP) and still use an indemnity policy to bridge the gap.
Costs and Policy Limitations
We often find that hospital indemnity is quite affordable, with some individual premiums starting as low as $10 to $20 per month. However, there are a few “gotchas” to watch out for:
- Waiting Periods: Some plans require you to be a member for 30 days before a claim is valid.
- Pre-existing Conditions: You might face exclusions if you seek care for a condition you had before the policy started.
- Guaranteed Issue: If you sign up during an employer’s open enrollment, you usually don’t have to answer medical questions. If you sign up later, you might.
Essential Documentation for Your hospital stay claim process
The secret to a fast hospital stay claim process is organization. If you send a half-finished form or a blurry photo of a receipt, your claim will likely hit a snag.
You will need a “superbill” or an itemized statement. A simple “Amount Due” notice isn’t enough. For a successful submission, ensure you have:
- Itemized Bills: These show every aspirin and X-ray with a corresponding code.
- Discharge Papers: These prove you were actually admitted and show the dates of your stay.
- Diagnosis Codes (ICD-10): These tell the insurer why you were there.
- Procedure Codes (CPT/HCPCS): These tell the insurer what was done.
- Proof of Stay: A signed statement from the facility confirming admission and discharge times.
For those using Medicare in the US, you’ll need to be familiar with the Patient Request for Medical Payment form (CMS-1490S). Students in Australia should keep similar records for their OSHC (Overseas Student Health Cover) providers. While providers usually file for you, knowing how to do it yourself is a vital backup skill. You can find More info about what documents students need for claims on our advisory pages if you are studying abroad and need to navigate international billing.
Organizing Records for a Smooth Submission
We recommend creating a “Claim Folder” (digital or physical) the moment you enter the hospital. Ask for the provider’s National Provider Identifier (NPI) and Tax ID number before you leave. If you are an international student, these details are often missing from standard receipts but are mandatory for the hospital stay claim process.
An explanatory letter can also help. If your stay was complicated, a brief summary of events can clear up confusion for the claims adjuster. Check out More info about how to effectively file a claim for our best tips on keeping your records audit-proof.
Step-by-Step Guide to the hospital stay claim process
Now, let’s get into the “how-to” of it all. Filing a claim isn’t just about dropping an envelope in the mail; it’s a multi-stage journey.
Initiating the hospital stay claim process
- Verify Benefits: Before filing, check your policy. Does it cover the specific reason for your stay?
- Log In: Most modern insurers have a member portal. This is almost always faster than mail.
- Fill the Form: Whether it’s a digital form or a paper one, be meticulous. Double-check your policy number.
- Upload Documents: Attach your itemized bills and discharge papers.
- Designate Payment: Decide if the money goes to you (the default for indemnity) or directly to the hospital (assignment of benefits).
For a deeper dive, read More info about the step-by-step guide to filing a claim.
Timelines for the hospital stay claim process
Patience is a virtue, but so is persistence. Most health plans in Australia and the US are legally required to notify you if a claim is accepted or denied within 30 business days. Many private insurers, like those we advise on, aim for a four-week turnaround.
However, you must be aware of the “statute of limitations” for claims:
- Medicare (US): You must file within 12 months (one full calendar year) of the service date.
- CHAMPVA: Claims must be filed within 1 year of the date of care or hospital discharge.
- Private Plans: These vary, but many give you 90 days to a year.
Don’t wait! The longer you wait, the harder it is to get the hospital to correct coding errors.
Managing Denials and Appeals in the Hospital Stay Claim Process
It happens to the best of us: you open your mail and see the words “Claim Denied.” Don’t panic. A denial is often just a request for more information.
Common reasons for a denial in the hospital stay claim process include:
- Coding Errors: The hospital used the wrong code for your procedure.
- Missing Information: You forgot to attach the discharge summary.
- Outpatient Status: You stayed overnight, but the hospital classified you as “under observation” (outpatient), which some indemnity plans don’t cover.
If you disagree with a decision, you have appeal rights. You can request a “decision review,” where a different adjuster looks at your file. If you are on Medicare in the US, you can seek SHIP (State Health Insurance Assistance Program) counseling for free help. In Australia, the Private Health Insurance Ombudsman offers support for students facing claim disputes. For students, we provide More info about how to file a travel insurance claim specifically tailored to handling common rejection reasons.
Frequently Asked Questions about Hospital Claims
Who receives the benefit payment?
In a traditional health insurance scenario, the provider gets paid. In the hospital stay claim process for an indemnity plan, the cash usually goes directly to you. This is a huge advantage. You can use the money for anything—household bills, childcare costs while you recover, or even high-quality groceries to help you get back on your feet. It is flexible spending at its finest.
How does this work with Medicare or Medicaid?
If you have Medicare in the US, your hospital stay is handled under Part A. In 2026, the Part A deductible is $1,736. If you stay longer than 60 days, you start paying coinsurance ($434/day for days 61–90). In Australia, international students rely on OSHC to cover the cost of hospital treatment and medical care. An indemnity plan can be used to pay deductibles or out-of-pocket gaps directly, saving you from dipping into your savings.
Can I keep my coverage if I change jobs?
Many employer-sponsored hospital indemnity plans are “portable.” This means if you leave your job, you can take the policy with you. You’ll just need to fill out a portability or continuation form and pay the premiums directly to the insurance company instead of through payroll deduction. This ensures you don’t have a gap in coverage during an employment transition.
Conclusion
At RecipesGuard, we know that being a student—especially one far from home—comes with enough challenges without adding medical debt to the mix. Navigating the hospital stay claim process is about being proactive, staying organized, and knowing your rights.
Whether you are looking for a student-focused guide on travel insurance or need a step-by-step tutorial on filing a complex claim, we are here to provide the financial security and clarity you need. By following these steps, you can focus on what really matters: your recovery and your education.
For more expert advice and tutorials, visit us at https://www.recipesguard.com/.