Why Every Student Needs to Understand the Medical Claim Process
A medical claim student guide can be the difference between getting fully reimbursed for a doctor visit and paying hundreds of dollars out of pocket. Whether you are studying at home in Australia or heading to the U.S. for an exchange program, understanding how to navigate insurance is a critical skill.
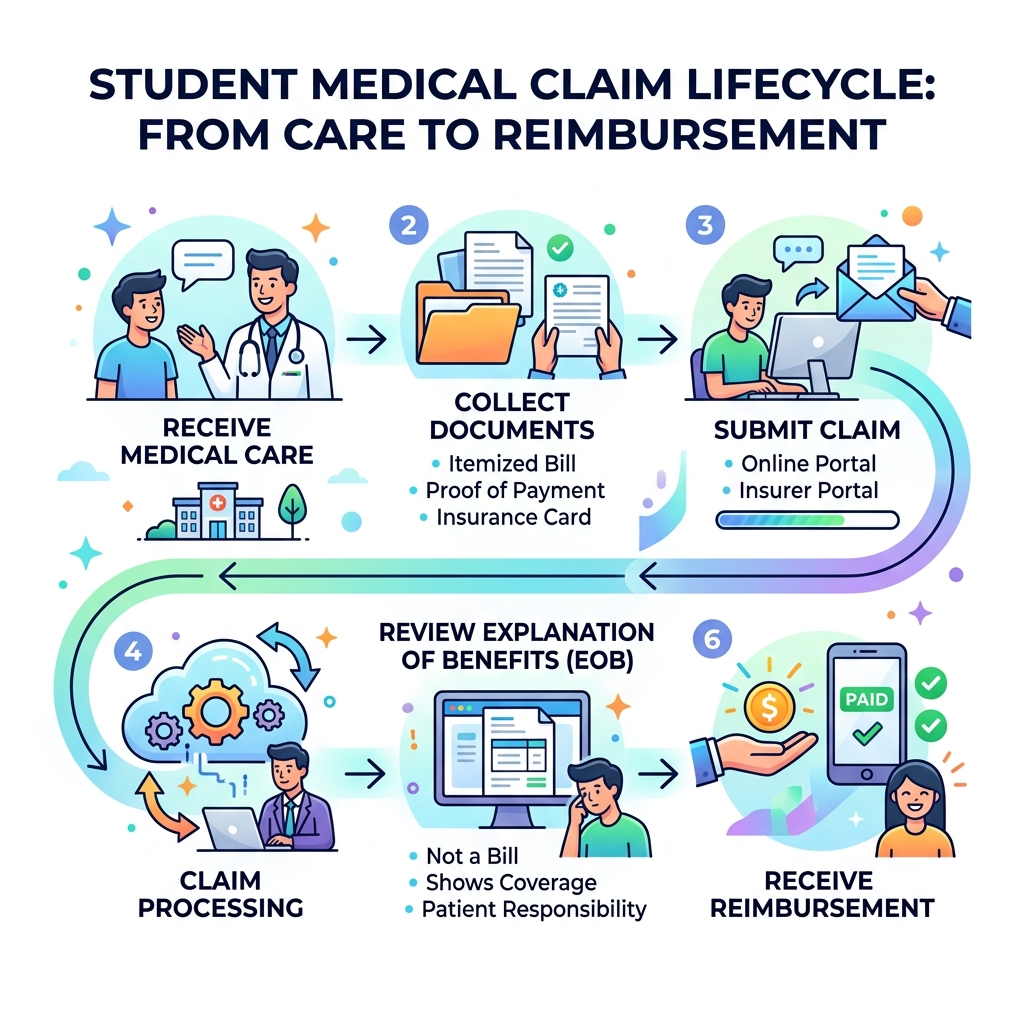
Here is a quick overview of how to file a student medical claim:
- Get care from a provider (in-network or out-of-network)
- Collect documents – itemized bill, proof of payment, and your insurance card
- Submit your claim – online portal, email, fax, or mail to your insurer
- Wait for processing – typically 14 to 60 days depending on submission method
- Review your EOB (Explanation of Benefits) – this is not a bill, just a breakdown of what your insurer covers
- Pay any remaining balance to your provider after insurance pays its share
Medical bills are confusing for anyone. For international students—such as Australians dealing with the unfamiliar U.S. healthcare system—they can feel overwhelming.
The truth is, most students don’t think about insurance claims until they’re already sitting in a waiting room – or worse, holding a bill they don’t understand.
In the U.S., where many Australian students travel for study, about 14% of college students are uninsured. Many more are underinsured or simply don’t know how to use their coverage. A single unplanned doctor visit can cost around $171 without insurance – and emergency care can run into thousands.
Whether you visited an in-network clinic or paid out of pocket at an out-of-network provider, the steps to get reimbursed follow a clear process. This guide walks you through every part of it – from filling out claim forms correctly to avoiding the most common mistakes that delay or deny payment.
Mastering the Medical Claim Student Guide for Reimbursement
When we talk about professional medical claims—especially for Australian students studying in the U.S.—the “gold standard” is the CMS-1500 form. This red-inked document is maintained by the National Uniform Claim Committee (NUCC). While it looks like a wall of boxes and numbers, it is the primary way healthcare providers tell insurance companies what they did and why they should be paid.
For students, understanding this form is vital because if you see an out-of-network provider, they might hand you a “superbill” or a partially completed CMS-1500 and tell you to “file it yourself.”
The CMS-1500 and ASCA Requirements
The Administrative Simplification Compliance Act (ASCA) generally requires that all claims be submitted to Medicare and other major insurers electronically. however, there are exceptions for small providers. If you are filing a paper claim, you must use an original, OMB-approved version of the CMS-1500 (currently version 02/12).
One of the biggest “gotchas” in any medical claim student guide is the photocopy rule: Never use a photocopy of the CMS-1500 form. The forms are printed in a special “drop-out” red ink so that high-speed scanners can read the data without seeing the lines. If you submit a black-and-white photocopy, the system will likely reject it immediately.
Electronic vs. Paper Submission
Electronic claims are the way to go whenever possible. They are processed faster—sometimes in as little as 14 business days—compared to the 30–60 days often required for paper claims. Most modern student health portals allow you to upload digital copies of your bills, which acts as an electronic submission.
When submitting data, insurers must follow the Federal Rules on Sharing Health Data to ensure your information moves securely between providers and payers.
Patient and Insured Details in Your Medical Claim Student Guide
Items 1 through 13 on the claim form focus on you—the patient. Accuracy here is non-negotiable. If your name is “Jonathan” on your insurance card but you write “Jon” on the claim, the computer might say “I don’t know this person” and kick the claim back.
- Item 1a: This is where you enter your Medicare Beneficiary Identifier (MBI) or your student insurance ID number.
- Item 3 (Date of Birth): This must follow an 8-digit format (MM | DD | CCYY). For example, if you were born on January 5, 2002, you would enter 01 05 2002.
- Gender Markers: You must select the gender that matches your insurance records.
- Item 11: This is a required field. By filling this out, you are acknowledging that you’ve made a good-faith effort to determine if another insurance plan should pay first. If you don’t have other insurance, you usually enter “NONE.”
Privacy is a big deal during this process. The U.S. Department of Health and Human Services HIPAA FAQs explain that your health data is protected, but you generally give “Signature on File” (SOF) permission in Items 12 and 13 so the insurer can process the payment and the provider can get paid.
Coding and Provider Info for Your Medical Claim Student Guide
Items 14 through 33 are the “technical” part of the claim. This is where the provider describes the medical necessity of your visit.
- NPI (National Provider Identifier): Every healthcare provider has a unique 10-digit NPI. You’ll see this in Items 17b, 24J, 32a, and 33a. Since 2008, NPIs have been mandatory—legacy IDs are no longer accepted.
- Diagnosis Codes (Item 21): This is where the “why” goes. Modern forms (02/12 version) allow for up to 12 diagnosis codes (labeled A-L). You must include an “ICD Indicator” to tell the system if you are using ICD-9 (rare now) or ICD-10 codes. (Hint: It’s almost always ICD-10, indicated by a ‘0’).
- Place of Service (POS) Codes: These two-digit codes tell the insurer where the service happened.
- POS 11: Office visit.
- POS 21: Inpatient hospital.
- POS 02 or 10: Telehealth.
The POS code is important because it dictates the payment rate. Medicare and other insurers use a “facility vs. non-facility” rate. Generally, services performed in a “non-facility” setting (like a private doctor’s office) pay a higher rate to the doctor to cover their overhead costs.
Step-by-Step Filing for In-Network and Out-of-Network Care
We know that navigating the difference between “in-network” and “out-of-network” feels like learning a second language, especially for Australian students used to a different healthcare model. Here is the breakdown:
In-Network Care: The “Easy” Way
If you go to a doctor who has a contract with your insurance, they usually do all the heavy lifting. You show your ID card, pay your copay (like the $25 fee common at many campus clinics), and walk out. The provider submits the claim directly to the insurer.
Out-of-Network Care: The “Manual” Way
If you see a specialist or go to a clinic outside your network, you might have to pay the full bill upfront. To get your money back, you need to follow our medical claim student guide steps:
- Request an Itemized Bill: A simple credit card receipt isn’t enough. You need a bill that includes CPT codes (what they did) and ICD-10 codes (why they did it).
- Verify Referrals: Some student plans require a referral from your school’s health center before you see a specialist. If you skip this, your claim might be denied.
- Proof of Payment: Keep your bank statement or the receipt showing the balance was paid in full.
- Submit via Portal: Most insurers (like Aetna, UHCSR, or Australian-based providers like Allianz Care) prefer you use their online “Member Account” or “My Account” portal. It’s faster and harder to lose than a paper envelope.
If you are traveling while studying, the process is similar but requires even more documentation. You can check out our Step-by-step guide to filing a travel insurance claim as a student for more specific tips on international scenarios.
Navigating Medicare Secondary Payer (MSP) Scenarios
Sometimes, you might be covered by more than one insurance policy. For example, an Australian student might have their own student health plan and still be a dependent on their parents’ plan (permitted until age 26 under the ACA in the U.S.).
In these cases, we have to deal with “Coordination of Benefits” (COB).
- Primary Payer: The insurance that pays the bill first.
- Secondary Payer: The insurance that covers the remaining balance (if any).
In Item 11 of the CMS-1500, you must indicate if there is another plan. If you are a student with a job that provides insurance, that might be primary, while your student plan becomes secondary. Following the Affordable Care Act (ACA) coverage rules, insurers work together to ensure they don’t pay more than 100% of the total bill.
If you are using Medicare, Item 11 is especially critical. You must acknowledge a “good faith effort” to determine if Medicare is the primary or secondary payer. This is common for students with certain disabilities or End-Stage Renal Disease who might be on Medicare while still in school.
Avoiding Common Errors and Claim Denials
Nothing is more frustrating than waiting 30 days for a check only to get a “Claim Denied” letter. Most rejections happen because of tiny, silly mistakes.
1. Incomplete Data
Missing a middle initial or a zip code can trigger a rejection. Ensure your address on file with the university matches the address on your claim.
2. Invalid NPI Numbers
If you are filling out the form yourself, double-check the doctor’s NPI. If the number is wrong or belongs to a different provider, the claim will be “invalid.”
3. Missing Signatures
In Items 12 and 13, you can often write “Signature on File.” However, if the insurer doesn’t actually have your signature on a master form, they can’t process the claim. Make sure you signed the initial HIPAA and consent forms at your doctor’s office.
4. Incorrect Place of Service (POS) Codes
If you had a telehealth visit from your dorm room but the claim says POS 11 (Office), it might be denied because the “facility fee” doesn’t match the service type.
5. NOC Codes in Item 19
If your doctor performed a procedure that doesn’t have a standard code (Not Otherwise Classified or NOC), they must explain it in Item 19. If this box is blank but an NOC code is used in Item 24, the claim will fail.
For those of us traveling abroad, emergency claims have even higher scrutiny. Understanding the nuances of medical emergency coverage in student travel insurance can help you ensure your “Item 19” notes are detailed enough to get approved.
Frequently Asked Questions about Student Medical Claims
What is an Explanation of Benefits (EOB)?
An EOB is the most misunderstood document in the medical claim student guide. It is not a bill. It is a report from your insurance company explaining:
- How much the doctor charged.
- The “allowed amount” (the discounted rate the insurer negotiated).
- How much the insurer paid.
- How much you still owe (your responsibility).
Always compare your EOB to the final bill you get from the doctor. If the doctor asks for $100 but the EOB says you only owe $20, call the doctor’s billing office!
How long do I have to submit my medical claim?
Timing is everything. Most student plans have a “timely filing” limit:
- In-Network: Providers usually must file within 90 to 120 days.
- Out-of-Network: You often have up to 12 months, but some plans are as strict as 90 days.
- International/UHCSR: Generally, you must submit within 90 days of the date of service.
If you miss the deadline, the insurer has the legal right to refuse payment entirely, leaving you with the full bill.
What documents count as “Proof of Payment”?
If you are asking for reimbursement, the insurance company needs to know you actually paid the money. Acceptable documents include:
- Itemized Receipt: Must show a $0.00 balance or “Paid in Full.”
- Bank/Credit Card Statement: A screenshot of the transaction (you can black out unrelated purchases).
- Cancelled Check: A scanned copy of the front and back of the check.
Knowing how to handle the hospital stay claim process is particularly helpful here, as hospital bills are often split into “hospital charges” and “physician charges,” requiring multiple proofs of payment.
Conclusion
At RecipesGuard, based in Australia, we believe that being a student is hard enough without having to moonlight as a medical billing expert. However, a little bit of knowledge goes a long way. By following this medical claim student guide, you can protect your bank account and ensure that your focus stays on your studies, not your debt.
Your Final Checklist:
- [ ] Did I use an original CMS-1500 (no photocopies)?
- [ ] Is my name and ID number exactly as they appear on my card?
- [ ] Did I use the 8-digit date format (MMDDCCYY)?
- [ ] Did I include the provider’s 10-digit NPI?
- [ ] Is my proof of payment attached?
If you’re feeling stuck or your claim was unfairly denied, don’t panic. You have the right to appeal. For more step-by-step tutorials and expert advice, you can always Get expert help with your student insurance claims. We are here to help you navigate the paperwork so you can get back to what matters most.