When Medical Bills Abroad Catch You Off Guard
The international student claim process is something most students never think about — until they’re sitting in an urgent care waiting room with a stack of unfamiliar paperwork and no idea what to do next.
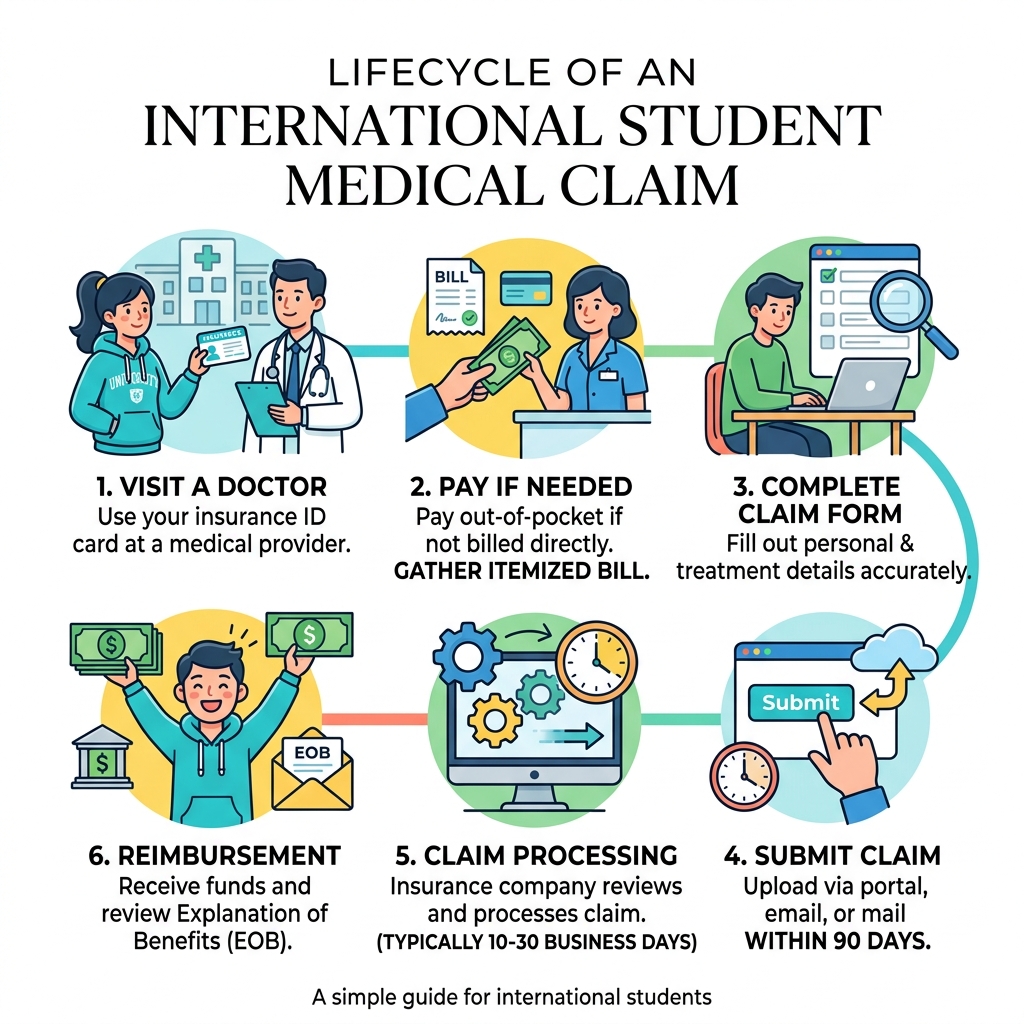
Here’s a quick overview of how the process works:
- Visit a doctor or medical provider (in-network or out-of-network)
- Pay out of pocket if your provider doesn’t bill your insurer directly
- Collect your itemized bill with service codes, diagnosis codes, and provider details
- Complete your insurer’s claim form with your personal, provider, and treatment information
- Submit your claim via online portal, email, fax, or mail — within 90 days of your visit
- Wait for processing — typically 10 to 30 business days depending on your insurer
- Review your Explanation of Benefits (EOB) to understand what was covered and what you owe
- Appeal if needed if your claim is denied or only partially approved
Most of the time, your healthcare provider handles billing directly with your insurance company. You just show your insurance ID card and walk out. But that doesn’t always happen — especially when you visit an out-of-network provider, pay cash, or deal with prescriptions, dental care, or specialist visits.
When direct billing falls through, knowing how to file a claim yourself can mean the difference between getting reimbursed and losing hundreds of dollars out of pocket.
This guide walks you through every step — from gathering documents to appealing a denied claim — so you can navigate the process with confidence.
Understanding the international student claim process
When we talk about the international student claim process, we are essentially describing the formal request you make to your insurance provider to cover the costs of your medical treatment. In a perfect world, you’d never have to touch a claim form. In the real world, especially for those of us studying in Australia or other popular destinations, the “manual claim” is a rite of passage.
What Exactly is a Health Insurance Claim?
Think of a claim as an invoice you send to your insurance company. It says, “Hey, I went to the doctor for a sore throat, it cost $80, and according to my policy, you should pay for this.” If the doctor sends this request themselves, it’s called direct billing. If you pay the $80 and then ask the insurance company to pay you back, it’s a reimbursement claim.
Direct Billing vs. Manual Reimbursement
In Australia, many Overseas Student Health Cover (OSHC) providers have “direct billing” arrangements with specific clinics. When you visit these “in-network” providers, you show your insurance ID card, pay any required copayment (your small share of the bill), and the clinic handles the rest.
However, if you end up at an “out-of-network” provider — perhaps the only clinic open at 2:00 AM — you will likely have to pay the full amount upfront. This is where the manual international student claim process kicks in.
| Feature | Direct Billing (In-Network) | Manual Reimbursement (Out-of-Network) |
|---|---|---|
| Upfront Cost | Usually just a small copay | Full cost of the visit |
| Paperwork | Minimal; handled by the clinic | You must collect and submit documents |
| Processing Time | Instant for you | 10–30 business days |
| Convenience | High | Moderate (requires follow-up) |
Key Terms to Know
- Provider Network: A list of doctors and hospitals that have a contract with your insurer. Staying “in-network” is the best way to avoid the headache of filing claims.
- Insurance ID Card: Your golden ticket. It contains your policy number and the contact info your doctor needs. Always keep a digital copy on your phone!
- Deductible: The amount you have to pay out of your own pocket before your insurance starts chipping in. If your deductible is $100 and your bill is $150, you pay the first $100, and the claim covers the remaining $50.

Essential Documentation for Your Claim
The number one reason the international student claim process gets delayed is missing paperwork. Insurance companies are notorious sticklers for detail. If your receipt doesn’t have the right “magic numbers,” they might send it back.
To ensure a smooth process, you should always check what documents students need for travel insurance claims before you leave the doctor’s office.
The Itemized Bill: The Holy Grail of Claims
A simple credit card receipt that says “Medical Clinic – $120” is not enough. You need an itemized bill. This is a detailed document that breaks down exactly what happened during your visit. It must include:
- Provider Information: The clinic’s name, address, and Tax ID (in Australia, this is often the ABN).
- Diagnosis Codes (ICD-10): These are international codes, maintained by the World Health Organization (WHO), that tell the insurer why you were there (e.g., “J02.9” for an unspecified sore throat).
- Procedure Codes (CPT or MBS): In Australia, these are often Medicare Benefit Schedule (MBS) item numbers. They tell the insurer exactly what the doctor did (e.g., a standard consultation).
- Service Date: Exactly when you were seen.
Proof of Payment
If you paid upfront, you need a receipt showing that the balance is $0. This proves you actually spent the money you’re asking back. If you haven’t paid yet but the provider won’t bill the insurer, you’ll submit the “unpaid” invoice so the insurer can pay the doctor directly.
Medical History and Records
Occasionally, for larger claims or accidents, the insurer might request your medical history. They want to see if the condition was “pre-existing.” While this sounds scary, it’s a standard part of the audit process for many international student policies. Keep a folder (digital or physical) with your records from back home just in case.
Step-by-Step Guide to Filing Your Claim
Ready to get your money back? We’ve broken down the international student claim process into four manageable steps. If you want to dive deeper into the nuances, we also have a guide on how to effectively file a travel insurance claim as a student.
Step 1: Collect Itemized Receipts
Don’t walk out of the clinic without that itemized bill! If you forgot it, call the provider’s billing department. Give them your name and the date of service, and ask them to email you a “detailed statement for insurance purposes.”
Step 2: Complete the Claim Form
Most insurers have a standard claim form. You can usually find this on their website or your university’s student portal. You will need to fill out:
- Personal Info: Your name, student ID, and current address in Australia.
- Provider Info: Who did you see?
- Reason for Visit: A brief description of your symptoms or the accident.
- Payment Instructions: Do you want a check mailed to you, or a direct deposit into your Australian bank account? (Pro tip: Direct deposit is much faster).
Step 3: Make Copies of Everything
This is the “Golden Rule” of the international student claim process. Before you hit send or drop anything in the mail, take a photo or scan every single page. If the mail gets lost or a file gets corrupted, you don’t want to have to start from scratch.
Step 4: Review and Submit
Double-check that your policy number is correct and that you’ve signed the form. You can typically submit via:
- Online Portals/Apps: Usually the fastest method.
- Email: Great for keeping a digital paper trail.
- Mail/Fax: Only use these if your insurer specifically requires them.
Important Deadline: Most claims must be submitted within 90 days of the service date. If you wait until the end of the semester to file all your receipts from February, you might find your claims denied simply because they are “stale.”
Navigating the Post-Submission Phase
Once you’ve clicked “submit,” the waiting game begins. But your job isn’t quite over yet. You need to monitor the progress to ensure nothing falls through the cracks.
Typical Processing Timelines
In our experience, most international student claims are processed within 10 to 30 business days.
- 10-20 days: Initial review and status update.
- 20-30 days: Final decision and payment issuance.
If you haven’t heard anything after 30 days, it’s time to be the “squeaky wheel.” Call the insurance hotline, have your claim reference number ready, and politely ask for an update. For a more detailed look at what happens during this wait, see our step-by-step guide to filing a travel insurance claim as a student.
Understanding Your Explanation of Benefits (EOB)
The EOB is one of the most confusing documents in the international student claim process. It is NOT a bill. It is a report card for your claim. It will show:
- Amount Billed: What the doctor charged.
- Plan Discount: The negotiated rate (if applicable).
- Amount Covered: What the insurance company paid.
- Patient Responsibility: What you still owe the doctor (or what was deducted from your reimbursement).
If the “Amount Covered” is $0, don’t panic yet. Look at the “Reason Code” or “Remarks” section. It might just mean they need more information, like a copy of your visa or a doctor’s note.
Handling Partial Approvals and Appeals
Sometimes an insurer will only pay part of a claim. This often happens if the doctor charged more than the “usual and customary” rate for that area. If you feel a denial was unfair, you have the right to appeal.
- Contact the insurer first: Sometimes a quick phone call can clear up a misunderstanding.
- Submit an Appeal Form: Most companies have a specific form for this.
- Provide Evidence: Get a letter from your doctor explaining why the treatment was medically necessary.
Special Considerations: From Prescriptions to Tax Refunds
The international student claim process isn’t just about doctor visits. There are several “special” types of claims you might encounter during your studies in Australia.
Prescriptions, Dental, and Vision
Many basic OSHC plans in Australia have limited coverage for “extras” like dental and optical.
- Prescriptions: You usually have to pay the full price at the pharmacy (chemist) and then claim back the amount that exceeds the current Pharmaceutical Benefits Scheme (PBS) co-payment rate.
- Dental/Vision: Check if you have “Extras” cover. If not, these will be entirely out-of-pocket unless they are part of an emergency hospital admission.
Emergency Room (ER) Visits
In Australia, if you are a “public” patient in a public hospital ER, your OSHC usually covers the cost. However, if you are admitted to a private hospital, the costs can skyrocket. Always try to go to a public hospital for emergencies unless your policy specifically lists private hospital cover.
Pre-approval for Specialists
If your GP refers you to a specialist (like a dermatologist or a surgeon), we highly recommend seeking pre-approval. This involves sending the specialist’s quote to your insurer before the appointment. They will tell you exactly how much they will cover, so you aren’t hit with a $500 surprise bill later.
The Other “Claim”: Tax Refunds
While not a medical claim, many students are surprised to learn they can claim money back from the government. If you’ve been working part-time in Australia, you’ve likely been paying income tax.
- Tax Returns: In Australia, the tax year ends on June 30. You can often file a tax return through the Australian Taxation Office (ATO) to get back overpaid tax.
- Tax Exemptions: Depending on your visa and residency status for tax purposes, you might be exempt from certain levies (like the Medicare Levy, since you already pay for OSHC).
Frequently Asked Questions about the international student claim process
What are common mistakes in the international student claim process?
We see the same errors over and over again. To avoid them, make sure you know how to file a travel insurance claim as a student correctly.
- Missing the 90-day deadline: This is the most common reason for denial.
- Incorrect Mailing Address: If you move house and don’t tell the insurer, your reimbursement check or EOB might end up in someone else’s mailbox.
- Forgetting Itemized Codes: A receipt without an MBS or ICD-10 code is just a piece of paper to an insurance adjuster.
- Not Keeping Copies: If the insurer says they never received your claim, and you don’t have a copy, you have no leverage.
How do I handle a denied or partially approved claim?
First, take a deep breath. A denial isn’t always the final word.
- Read the EOB: Look for the specific reason code.
- Call the Hotline: Ask for a detailed explanation. Sometimes it’s just a clerical error.
- Visit Your International Student Office: Many universities have staff dedicated to helping students navigate insurance issues.
- File a Formal Appeal: Include a written statement and any new medical evidence.
When is pre-approval required for medical services?
You should seek pre-approval for any non-emergency service that is likely to be expensive. This includes:
- Specialist consultations and diagnostic tests (like MRIs).
- Planned surgeries or hospital stays.
- Durable medical equipment (like crutches or braces).
- Psychological counseling or long-term therapy.
Seeking pre-approval usually takes 3-5 business days, but it provides immense peace of mind.
Conclusion
Navigating the international student claim process doesn’t have to be a nightmare. By staying organized, keeping meticulous records, and understanding the “rules of the game,” you can ensure that you get every cent you’re entitled to.
At RecipesGuard, we specialize in providing student-focused tutorials that take the mystery out of insurance. Whether you’re dealing with a simple GP visit or a complex specialist referral, you have resources available to you. Utilize your university’s health services, call your insurance provider’s multilingual support lines, and don’t be afraid to ask questions.
Don’t let medical bills distract you from your studies and your adventures abroad. Start your claim journey today and take control of your financial health while studying overseas. Safe travels and stay healthy!